Fungal Acne on Back and Chest
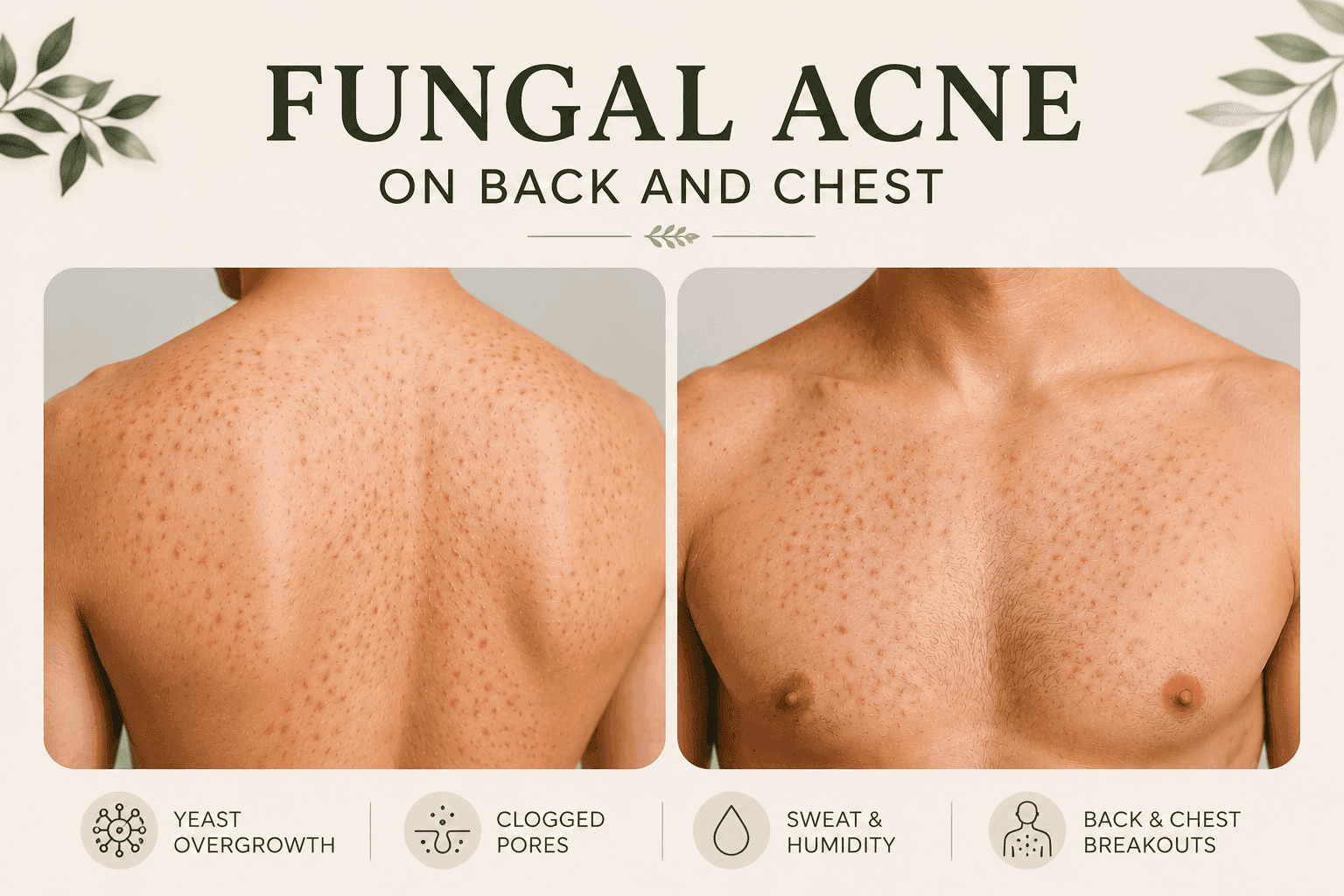
Fungal acne on the back and chest is not true acne — it is a yeast infection of the hair follicles called pityrosporum folliculitis (also known as Malassezia folliculitis). It produces small, uniform, itchy bumps triggered by heat, sweat, and occlusive skincare products. Unlike bacterial acne, it does not respond to benzoyl peroxide or antibiotics. Antifungal interventions, moisture control, and avoiding yeast-feeding ingredients are the core of effective management.
Pityrosporum folliculitis (also called Malassezia folliculitis) is a fungal skin condition in which yeast overgrowth inside hair follicles causes small, itchy bumps on the back, chest, and shoulders. The causative organism — Malassezia — lives naturally on all human skin but overgrows when warmth, moisture, and sebum create favourable conditions [1].
At a glance:
- Cause: Malassezia yeast overgrowth inside hair follicles
- Location: Upper back, chest, shoulders — areas with dense sebaceous glands
- Key symptom that separates it from bacterial acne: intense itch that worsens with heat
- What makes it worse: sweat, antibiotics, occlusive products, fatty-acid-rich ingredients
- What actually works: antifungal approaches, moisture control, fungal-acne-safe product swaps
Fungal acne on the back and chest appears as small, uniform bumps that often itch and worsen with heat or sweat. Unlike bacterial acne, it's caused by an overgrowth of yeast that lives naturally on your skin, triggered by moisture, occlusion, and disrupted skin microbiome balance.
Key Takeaways:
- Fungal acne is not true acne but a yeast infection called pityrosporum folliculitis
- It thrives in warm, moist environments and appears as itchy, uniform bumps
- Common triggers include sweaty clothing, occlusive products, and antibiotics
- Traditional acne treatments often make it worse
- Managing moisture and restoring skin balance are essential
What Fungal Acne Actually Is
Fungal acne is a misleading name. The bumps on your back and chest aren't caused by the same bacteria responsible for traditional acne. Instead, they result from pityrosporum folliculitis, an overgrowth of Malassezia yeast inside your hair follicles. This yeast exists naturally on everyone's skin as part of the normal microbiome. Problems begin when conditions allow it to multiply beyond normal levels.
The yeast feeds on oils and thrives in warm, humid environments. When it overgrows, it triggers inflammation inside the follicle, creating small, itchy bumps that look remarkably similar to acne. The body recognizes this overgrowth as an irritant and responds with an immune reaction.
Why Your Back and Chest Are Vulnerable
The back and chest create ideal conditions for yeast overgrowth due to high sebum production and frequent occlusion from clothing.
Sweat, friction, and synthetic fabrics trap heat and moisture, creating a microenvironment where Malassezia thrives. Body lotions and sunscreens containing fatty acids (like coconut oil or shea butter) can further feed the yeast.
How Fungal Acne Differs From Bacterial Acne
Bacterial acne includes comedones, pustules, and cysts of varying sizes. Fungal acne presents as uniform, small bumps that often itch intensely.
Key differences:
- Fungal acne itches; bacterial acne usually does not
- Fungal acne bumps are uniform; bacterial acne varies in size
- Fungal acne worsens with heat and sweat
- Antibiotics worsen fungal acne
Ingredients That Feed Malassezia — and What to Use Instead
Malassezia depends on external lipids to survive [2].
Ingredients to avoid:
| Ingredient | Found in | Why it's problematic |
|---|---|---|
| Shea butter | Lotions | Oleic acid source |
| Coconut oil | Oils, hair products | Lauric acid feeds yeast |
| Fatty alcohols | Moisturisers | Lipid source |
| Esters | Sunscreens | Break down into fatty acids |
| Squalane (olive-derived) | Serums | Oleic acid content |
| Polysorbates | Emulsifiers | Release fatty acids |
| Oleic acid | Oils | Direct yeast fuel |
Safer ingredients:
- Zinc pyrithione
- Ketoconazole
- Niacinamide
- Hyaluronic acid
- Glycerine
- Sugarcane-derived squalane
- Azelaic acid
- Sulfur
Fungal Acne vs Other Conditions
| Feature | Fungal Acne | Bacterial Folliculitis | Keratosis Pilaris |
|---|---|---|---|
| Cause | Yeast | Bacteria | Keratin buildup |
| Itch | Strong | Mild/painful | Mild |
| Appearance | Uniform bumps | Mixed lesions | Rough texture |
| Antibiotics | Worsen | Improve | No effect |
| Antifungals | Improve | No effect | No effect |
Common Triggers
- Antibiotic use
- Humid climates
- Stress and cortisol changes
- High sugar intake
- Occlusive skincare products
- Sweaty clothing left on skin
What Happens Inside the Skin
Malassezia overgrowth triggers inflammation inside the follicle. Immune response leads to swelling, blockage, and formation of small itchy bumps.
Research Summary
Key findings:
- Malassezia thrives on C11–C24 fatty acids [2]
- Ketoconazole and itraconazole are effective treatments [3]
- Antibiotics often worsen fungal acne by disrupting microbiome balance
Why Traditional Acne Treatments Don’t Work
- Benzoyl peroxide targets bacteria, not yeast
- Retinoids affect cell turnover, not fungal growth
- Antibiotics worsen yeast overgrowth
Early Signs
- Sudden appearance of small bumps
- Intense itching
- Symmetrical distribution
- Worsening after sweat or heat exposure
Habits That Make It Worse
- Staying in sweaty clothes
- Sharing towels
- Hot long showers
- Heavy occlusive skincare
What Helps First
- Shower within 30 minutes after sweating
- Wear breathable fabrics
- Reduce oily skincare products
- Wash bedding regularly
Treatment Approach
Step 1: Remove moisture exposure
Change out of sweaty clothing quickly and avoid prolonged damp skin contact.
Step 2: Remove triggering products
Avoid fatty acids, esters, and oil-based products.
Step 3: Antifungal cleansing
Use ketoconazole or zinc pyrithione body wash.
Step 4: Fabric changes
Use breathable clothing and avoid synthetic tight fabrics.
Step 5: Haircare adjustment
Keep conditioner off the back and shoulders.
Step 6: Monitor progress
If no improvement in 4 weeks, consult a dermatologist.
Timeline
| Time | Progress |
|---|---|
| Week 1 | Reduced itching |
| Week 2 | Fewer new bumps |
| Week 3–4 | Flattening begins |
| Week 4–8 | Significant clearing |
Skin Barrier Support
- Gentle cleansing
- Avoid harsh soaps
- Maintain hydration
- Avoid over-exfoliation
When to See a Dermatologist
- No improvement after 4 weeks
- Painful or spreading lesions
- Possible secondary infection
Frequently Asked Questions
Can ketoconazole shampoo be used?
Yes, it is commonly used off-label as a body wash.
Is niacinamide safe?
Yes, it does not feed Malassezia.
Does diet affect fungal acne?
Indirectly, through inflammation and oil production.
Will it leave scars?
Usually only temporary pigmentation, not scars.
Can I work out?
Yes, but shower soon after.
What This Means for You
Most people with fungal acne on their back and chest see a measurable reduction in itching within one to two weeks of controlling moisture and switching to fungal-acne-safe products. Visible clearing of bumps typically follows within four to eight weeks when an antifungal cleansing step is added consistently. Recurrence is common if the triggering conditions return — but with the right habits in place, flare-ups become shorter and less severe each time.
Your next actions:
- Audit body lotions, sunscreens, and haircare products and remove fatty-acid-heavy ingredients
- Start zinc pyrithione or ketoconazole 2% body wash (leave for 3 minutes)
- Change out of sweaty clothing within 30 minutes
- Seek dermatology help if hormonal or internal triggers persist
- Consult a dermatologist if no improvement after 4 weeks
If environmental and product changes are not enough, deeper internal factors like hormones, stress, or gut imbalance may be contributing and may require structured skin assessment.
Editorial Standards
Clear Ritual has Strict sourcing guidelines to ensure our content is accurate and current. We rely on peer-reviewed studies, academic research institutions, and medical associations. We strive to use primary sources and refrain from using tertiary references. See a mistake? Learn More about our Editorial Standards.
Related Articles
Antibiotics and Fungal Acne: Understanding the Link
Published June 6, 2026

Forehead Acne vs Fungal Acne: Differences in Causes and Treatment
Published May 26, 2026
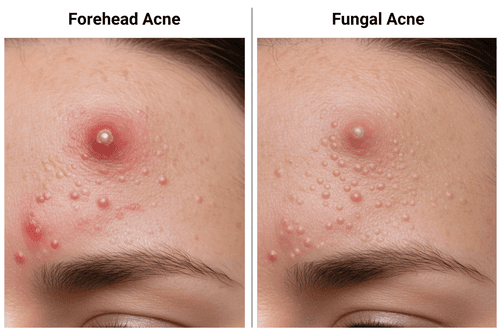
Do You Have Fungal Acne? Here's How It's Different From Bacterial Breakouts
Published May 26, 2026

Fungal Acne: Causes, Symptoms, Treatment & Prevention Tips
Published May 26, 2026


