Antibiotics and Fungal Acne: Understanding the Link

If you've noticed small, uniform bumps appearing on your forehead, cheeks, or chest after taking antibiotics, you might be dealing with fungal acne. Antibiotics disrupt the skin's natural microbiome by killing beneficial bacteria, which allows yeast to overgrow in hair follicles, creating inflamed bumps that resist typical acne treatments.
Key Takeaways:
- Fungal acne appears as clusters of small, itchy bumps that look similar but aren't bacterial acne
- Antibiotics kill both harmful and protective bacteria, allowing yeast overgrowth
- The condition occurs when Malassezia yeast multiplies inside hair follicles
- Traditional acne treatments often worsen fungal acne
- Restoring skin microbiome balance is essential for resolution
What Is Fungal Acne
Fungal acne, clinically called Malassezia folliculitis, develops when yeast naturally present on everyone's skin multiplies excessively inside hair follicles. Unlike bacterial acne where Cutibacterium acnes bacteria trigger inflammation in clogged pores, fungal acne involves yeast feeding on sebum and creating uniform inflammatory bumps.
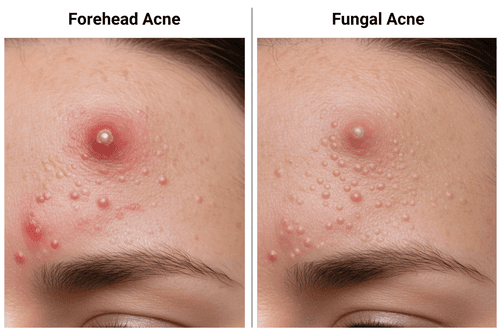
These bumps typically measure one to two millimeters, appear in clusters, and feel itchy rather than painful. They commonly show up on the forehead, temples, chest, shoulders, and back where sebaceous glands produce more oil. The uniformity distinguishes them from bacterial acne, which features varying sizes of comedones, papules, and pustules.
How Antibiotics Trigger Fungal Overgrowth
Your skin hosts a complex ecosystem of bacteria, fungi, and other microorganisms that maintain balance through competition for resources and space. This microbial community forms your skin's protective barrier against harmful pathogens.
When you take oral antibiotics for acne, respiratory infections, or other conditions, these medications travel through your bloodstream and reach your skin. Antibiotics cannot distinguish between beneficial and harmful bacteria, so they eliminate both. Common antibiotics like doxycycline, minocycline, and tetracycline prescribed for acne significantly reduce bacterial populations on your skin.
This bacterial reduction creates an opportunity for Malassezia yeast. Without bacterial competitors consuming sebum and occupying follicular space, yeast populations expand rapidly. Malassezia thrives in lipid-rich environments, and your sebaceous follicles provide ideal conditions with constant sebum production, warm temperatures, and reduced bacterial competition.
The overgrowth typically emerges two to four weeks after starting antibiotic therapy, though timing varies based on antibiotic type, dosage, duration, and individual microbiome composition.
The Skin Microbiome Disruption Cycle
Healthy skin maintains approximately one million bacteria per square centimeter, with Staphylococcus epidermidis and other beneficial species dominating the landscape. These bacteria produce antimicrobial peptides that suppress pathogenic organisms, regulate inflammation, and support barrier function.
Antibiotic therapy depletes these protective populations. As beneficial bacteria decline, several changes occur simultaneously. Sebum accumulates without bacterial processing, creating more yeast food. Skin pH shifts because bacteria normally produce acids that maintain optimal conditions. The immune system loses bacterial signals that calibrate appropriate inflammatory responses.
Malassezia yeast, naturally present at lower levels, recognizes this ecological void and proliferates. The yeast secretes enzymes that break down triglycerides in sebum into free fatty acids. These fatty acids irritate follicle walls, triggering inflammation that manifests as the characteristic bumps.
The inflammation differs from bacterial acne. While bacterial acne involves neutrophils attacking bacteria in blocked pores, fungal acne triggers lymphocytic inflammation responding to yeast byproducts. This explains why benzoyl peroxide and salicylic acid, which target bacteria and exfoliate dead cells, fail to improve fungal acne and sometimes worsen it by further disrupting the microbiome.
Recognizing Fungal Acne Versus Bacterial Acne
Understanding the differences helps you identify when antibiotics might be contributing to your skin concerns rather than resolving them.
| Feature | Bacterial Acne | Fungal Acne |
|---|---|---|
| Appearance | Varied sizes, comedones, cysts | Uniform small bumps |
| Sensation | Tender or painful | Itchy |
| Distribution | Random, scattered | Clustered patterns |
| Location | Face, jawline | Forehead, chest, back |
| Response to Treatment | Improves with antibiotics | Worsens with antibiotics |
Fungal acne creates monomorphic lesions, meaning they look remarkably similar in size and appearance. If you notice your skin developing dozens of identical small bumps while taking antibiotics for what you thought was regular acne, fungal overgrowth deserves consideration.
The itching provides another important clue. Bacterial acne rarely itches unless severely inflamed or healing. Fungal acne often creates persistent itching because yeast metabolic byproducts irritate nerve endings in follicle walls.
Common Scenarios That Increase Risk
Several situations combine antibiotic exposure with other factors that favor yeast proliferation, creating perfect conditions for fungal acne development.
Long-term antibiotic use for acne creates the most common scenario. Dermatologists sometimes prescribe months of oral antibiotics to control inflammatory acne. While this approach reduces acne bacteria initially, extended use progressively depletes protective bacterial populations and allows yeast to establish dominance.
Hot, humid environments accelerate the process. Sweating increases follicular moisture and warmth, both of which Malassezia yeast prefers. If you live in tropical climates or experience hot summers while taking antibiotics, your risk increases substantially. Occlusive clothing that traps sweat against your skin compounds the problem.
High-carbohydrate diets may contribute by increasing sebum production and altering its composition. While yeast feeds primarily on skin surface lipids rather than blood sugar, metabolic changes from sustained high glucose intake affect sebum quality and potentially create more favorable conditions for yeast metabolism.
Stress elevates cortisol, which increases oil production and suppresses certain immune functions that normally control yeast populations. If you started antibiotics during a stressful period and maintain high stress levels, your body's ability to restore microbial balance diminishes.
Skincare products containing oils and fatty acids feed Malassezia directly. Ingredients like coconut oil, olive oil, and certain fatty acid esters provide exactly what yeast needs to thrive. Continuing these products while your bacterial populations recover from antibiotic exposure sustains the overgrowth.
The Barrier Function Connection
Your skin barrier comprises corneocytes held together by lipid layers containing ceramides, cholesterol, and fatty acids. This structure prevents water loss and blocks external irritants and pathogens.
The microbiome contributes to barrier health by training immune cells, producing beneficial metabolites, and competing with harmful organisms. When antibiotics disrupt bacterial communities, barrier function can decline even if you don't develop visible fungal acne.
Reduced barrier function increases transepidermal water loss, which triggers compensatory sebum production. More sebum means more yeast food. Additionally, compromised barriers allow deeper penetration of yeast byproducts, intensifying inflammation and creating more noticeable symptoms.
This explains why some people develop fungal acne quickly after starting antibiotics while others remain clear despite similar treatments. Individual barrier strength, baseline microbiome diversity, genetic factors affecting immune responses, and environmental exposures all influence susceptibility.
Early Warning Signs
Recognizing fungal acne early allows faster intervention before overgrowth becomes established and difficult to reverse.
The first sign often appears as subtle texture changes rather than visible bumps. Your forehead or chest might feel slightly rough when you run your fingers across the skin. Small flesh-colored or slightly red bumps emerge next, usually in concentrated areas rather than randomly distributed.
Itching develops as yeast populations expand. The itching typically feels different from dry skin itching, more persistent and localized to areas with visible bumps. You might notice the itching worsens after sweating or applying moisturizers.
Lack of response to your usual acne treatments provides another clue. If you've been using benzoyl peroxide or salicylic acid successfully and suddenly these products stop working or your skin appears worse, consider whether recent antibiotic use might have shifted your skin ecology toward fungal predominance.
Pay attention to timing. If new bumps appeared within weeks of starting oral antibiotics and don't respond to topical acne medications, fungal overgrowth becomes more likely than coincidental bacterial acne worsening.
What Helps Restore Balance
Addressing antibiotic-related fungal acne requires stopping the overgrowth while supporting microbiome recovery. This differs fundamentally from treating bacterial acne.
First, evaluate whether continuing antibiotics serves your overall health needs. If you're taking antibiotics for acne and suspect fungal overgrowth, consult your healthcare provider about discontinuing or switching approaches. If antibiotics treat another condition, discuss the timeline and whether probiotics might help, though oral probiotics affect gut rather than skin microbiomes directly.
Reduce yeast food sources by temporarily avoiding skincare products with oils and fatty acid esters. Check ingredient lists for coconut oil, olive oil, squalene, and fatty alcohols. Simple, oil-free cleansers and lightweight gel moisturizers minimize yeast nutrition during recovery.
Manage moisture and occlusion carefully. Shower promptly after sweating to remove the combination of moisture, warmth, and sebum that yeast prefers. Choose breathable fabrics that don't trap sweat against your skin. If you wear hats or headbands regularly, clean them frequently to prevent yeast accumulation.
Support your skin barrier with ingredients that strengthen without feeding yeast. Hyaluronic acid provides hydration without lipids. Niacinamide reduces oil production, calms inflammation, and supports barrier function through multiple mechanisms. Ceramides in specific formulations help restore barrier lipids that don't promote yeast growth.
Give your microbiome time to rebalance. Bacterial populations recover gradually after antibiotic cessation, typically requiring several weeks to months for full restoration. Avoid introducing new harsh treatments that might further disrupt recovery. Gentle, consistent routines work better than aggressive interventions.
When Professional Guidance Becomes Necessary
While understanding fungal acne helps you make informed decisions, certain situations require dermatological evaluation.
Seek professional help if bumps persist beyond six weeks after stopping antibiotics. Extended persistence suggests either established overgrowth requiring specific treatment or misidentification of the condition. Dermatologists can perform simple tests to confirm Malassezia involvement.
Worsening symptoms despite stopping antibiotics and adjusting skincare indicate the need for assessment. Severe itching, spreading beyond initial areas, or development of painful nodules warrant prompt evaluation.
If you cannot discontinue antibiotics due to other medical needs but continue developing new fungal acne lesions, dermatologists can recommend approaches that address both your underlying condition requiring antibiotics and the secondary fungal overgrowth.
Uncertainty about whether you're experiencing fungal acne, bacterial acne, or another condition justifies consultation. Attempting to self-treat the wrong condition wastes time and potentially worsens your skin. Dermatologists distinguish between similar-appearing conditions through clinical examination and sometimes simple laboratory tests.
Prevention During Antibiotic Therapy
If you must take antibiotics for medical reasons, certain strategies may reduce fungal acne risk, though no approach guarantees prevention.
Maintain a simple skincare routine without heavy oils or occluding products. This reduces available nutrition for opportunistic yeast even as bacterial populations decline. Choose non-comedogenic, oil-free formulations for all skincare steps.
Manage environmental factors within your control. Keep skin as dry as possible by showering after exercise, using absorbent fabrics, and avoiding prolonged exposure to hot, humid conditions when feasible.
Consider the shortest effective antibiotic duration for your condition. Discuss with your prescribing physician whether shorter courses might achieve therapeutic goals while minimizing microbiome disruption.
Monitor your skin for early changes. Catching subtle signs early allows faster adjustment of your routine before overgrowth becomes established and symptomatic.
The Recovery Timeline
Understanding realistic expectations helps reduce frustration during the healing process.
After removing factors supporting yeast overgrowth, visible improvement typically begins within two to three weeks. Existing bumps gradually flatten as inflammation subsides and yeast populations decline. Itching usually resolves before visible changes occur.
Complete clearance generally requires four to eight weeks, depending on overgrowth severity, how quickly your microbiome rebalances, and whether you've eliminated all contributing factors. Some people clear faster, others slower, based on individual variation in immune function and microbial resilience.
Occasional bumps might appear during recovery as yeast populations fluctuate. This doesn't necessarily indicate treatment failure but rather the dynamic process of ecosystem rebalancing. Consistent supportive care typically leads to progressive improvement despite minor setbacks.
Skin texture normalizes last. Even after bumps disappear, subtle roughness might persist for weeks as follicles fully heal and surface cell turnover returns to normal patterns.
Understanding Internal Triggers: Clear Ritual's Perspective
Fungal acne demonstrates how skin conditions arise from multiple interacting factors rather than single causes. While antibiotic-triggered microbiome disruption creates the immediate problem, underlying factors like sebum production, barrier function, immune regulation, and environmental exposures all influence whether and how severely fungal overgrowth develops.
Addressing visible symptoms provides relief, but understanding your individual pattern of triggers supports long-term skin stability. At Clear Ritual, we combine the best of three worlds - Ayurveda, modern dermatology, and advanced skin science - to understand individual triggers through a structured Clear Ritual Skin Test. This approach recognizes that identical symptoms in different people may stem from different underlying imbalances requiring personalized attention.
Sustainable skin health comes from identifying your specific combination of internal and external factors, then supporting your skin's natural resilience rather than merely suppressing individual symptoms as they appear.
Frequently Asked Questions
Can antibiotics cause fungal acne even if I've never had acne before?
Yes, antibiotics disrupt the skin microbiome regardless of previous acne history. Anyone taking oral antibiotics can develop fungal acne if yeast populations overgrow in the altered microbial environment. Your baseline skin type and microbiome composition influence susceptibility, but prior acne isn't necessary for antibiotic-related fungal overgrowth to occur.
How long after starting antibiotics does fungal acne typically appear?
Most people notice fungal acne symptoms two to four weeks after beginning antibiotic therapy. The timeline varies based on antibiotic type, dosage, treatment duration, and individual factors like baseline microbiome diversity and sebum production. Some people develop symptoms within days, while others require months of antibiotic exposure before yeast overgrowth becomes symptomatic.
Will fungal acne go away on its own after stopping antibiotics?
Fungal acne often improves gradually after discontinuing antibiotics as bacterial populations recover and restore competitive balance. However, resolution isn't guaranteed without additional support. Removing yeast-feeding ingredients from skincare, managing moisture, and supporting barrier function typically accelerate clearing compared to simply waiting after antibiotic cessation.
Can I use acne spot treatments on fungal acne bumps?
Traditional acne spot treatments containing benzoyl peroxide or salicylic acid don't effectively address fungal acne and may worsen it by further disrupting the microbiome and irritating already inflamed follicles. These ingredients target bacteria and exfoliate dead cells but don't affect yeast overgrowth. Simple, gentle care works better than active spot treatments for fungal acne.
Does diet affect fungal acne the same way it affects bacterial acne?
Diet influences fungal acne differently than bacterial acne. While high-glycemic foods may increase sebum production that feeds yeast, Malassezia doesn't respond directly to blood sugar levels the way insulin and hormones affect bacterial acne. Reducing sebum production through balanced nutrition may help, but dietary changes alone rarely resolve established fungal overgrowth without addressing microbiome imbalance.
Can I prevent fungal acne if I must take antibiotics long-term?
Complete prevention during extended antibiotic therapy proves difficult since microbiome disruption continues throughout treatment. However, using oil-free skincare, managing moisture and occlusion, maintaining barrier health, and monitoring for early signs allow faster intervention if overgrowth begins. Some people tolerate long-term antibiotics without developing fungal acne due to individual microbiome resilience.
Is fungal acne contagious or can it spread to other body areas?
Fungal acne isn't contagious because it results from overgrowth of yeast already present on everyone's skin rather than infection from external sources. It can spread to other areas of your own body where conditions favor yeast proliferation, particularly sebum-rich areas like the chest, back, and shoulders. Addressing the underlying microbiome imbalance prevents spreading better than treating individual areas.
How can I tell if my skin is improving or if new bumps mean treatment isn't working?
Improvement shows as reduced itching, fewer new bumps appearing, and gradual flattening of existing bumps. Some fluctuation during recovery is normal as yeast populations decline unevenly. Consistent worsening with increasing bumps, spreading to new areas, or intensifying itching suggests your current approach needs adjustment or professional evaluation to confirm the diagnosis.
Editorial Standards
Clear Ritual has Strict sourcing guidelines to ensure our content is accurate and current. We rely on peer-reviewed studies, academic research institutions, and medical associations. We strive to use primary sources and refrain from using tertiary references. See a mistake? Learn More about our Editorial Standards.