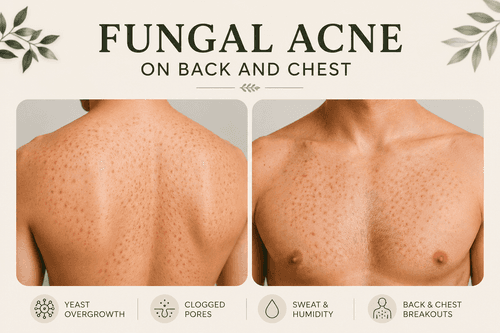
Fungal Acne in Humid and Tropical Weather

If you've noticed small, uniform bumps across your forehead, chest, or back that don't respond to typical acne treatments, especially during hot and humid months, you may be dealing with fungal acne. Unlike bacterial acne, fungal acne is caused by an overgrowth of yeast that thrives in warm, moist environments, making it particularly common in tropical climates.
Key Takeaways:
- Fungal acne is not true acne but a yeast overgrowth in hair follicles
- Heat, humidity, and sweating create ideal conditions for yeast proliferation
- It appears as small, itchy, uniform bumps that don't respond to standard acne treatments
- Breathable clothing, proper hygiene timing, and barrier support help manage symptoms
- Traditional acne products may worsen fungal acne by disrupting skin balance
What Fungal Acne Actually Is
Fungal acne, medically known as pityrosporum folliculitis or malassezia folliculitis, occurs when yeast organisms that naturally live on your skin multiply excessively inside hair follicles. This overgrowth triggers inflammation and creates clusters of small, itchy bumps that mimic bacterial acne but behave differently.
The condition results from an imbalance in your skin's microbiome. Under normal circumstances, yeast, bacteria, and other microorganisms coexist peacefully on your skin surface. When conditions shift in favor of yeast proliferation, these organisms move deeper into follicles, where they feed on sebum and trigger an inflammatory response.
Unlike bacterial acne, which forms comedones, cysts, or pustules of varying sizes, fungal acne presents as monomorphic lesions. These bumps appear remarkably uniform in size and shape, often covering large areas like the forehead, temples, chest, shoulders, or upper back. The affected areas typically feel itchy, a symptom rarely associated with bacterial acne.
Why Humid and Tropical Climates Trigger Fungal Acne
Malassezia yeast thrives in environments that combine three elements: warmth, moisture, and lipids. Tropical and humid climates provide all three conditions simultaneously, creating a perfect breeding ground for yeast overgrowth.
When environmental humidity exceeds 60 percent, sweat evaporation slows dramatically. This means moisture lingers on your skin surface longer, creating a damp environment against your follicles. The warmth of tropical climates accelerates sebum production, providing abundant food for yeast organisms. As temperatures rise, your sebaceous glands increase oil output to compensate for potential moisture loss, inadvertently fueling yeast growth.
The interaction between sweat and sebum creates an occlusive layer on skin. When this mixture sits against follicle openings for extended periods, it traps heat and moisture while blocking normal airflow. Yeast populations multiply rapidly in these oxygen-poor, lipid-rich pockets.
Seasonal patterns often reveal this relationship clearly. People living in regions with distinct wet and dry seasons frequently notice fungal acne flares during monsoon months or summer humidity peaks, with improvement during drier periods when moisture levels drop and sweat evaporates more efficiently.
How Daily Habits Worsen the Condition
Certain routine behaviors create microenvironments that accelerate yeast proliferation, often without your awareness. Wearing tight synthetic fabrics during humid weather traps sweat against your skin, preventing evaporation and creating sustained moisture exposure. Athletic wear made from non-breathable materials becomes particularly problematic during workouts, when sweat production peaks.
Delaying showers after sweating allows the sweat-sebum mixture to sit against follicles for extended periods. Even a two-hour delay between exercise and cleansing gives yeast substantial time to multiply. Similarly, sleeping in clothes you've worn throughout a humid day transfers accumulated sweat, oils, and yeast back onto your skin throughout the night.
Heavy moisturizers and occlusive skincare products create barriers that trap heat and moisture beneath them. Formulations containing oils, fatty acids, or esters that yeast feeds upon directly fuel overgrowth. Many conventional skincare products designed for dry skin contain these exact ingredients, making them counterproductive in humid climates prone to fungal acne.
Using harsh cleansers or over-washing disrupts your skin's protective barrier and alters pH levels. This damage doesn't eliminate yeast but instead removes competing bacteria, allowing yeast to dominate the disrupted microbiome. The resulting imbalance often worsens fungal acne despite increased cleansing frequency.
What Happens Inside Your Skin
Understanding the physiological process helps explain why fungal acne behaves so differently from bacterial acne. Malassezia yeast produces lipases, enzymes that break down triglycerides in sebum into free fatty acids. These free fatty acids serve as yeast food while simultaneously triggering inflammation in surrounding tissue.
As yeast populations expand within follicles, they provoke an immune response. Your skin recognizes the overgrowth as abnormal and sends inflammatory signals to the area. This inflammation causes the characteristic redness, swelling, and itching associated with fungal acne. Unlike bacterial acne, where bacteria create true infection, fungal acne represents an inflammatory reaction to overgrowth rather than infection.
The follicular environment becomes increasingly hospitable to yeast as this cycle continues. Inflammation damages the follicle lining, increasing sebum leakage into surrounding tissue. This leaked sebum provides additional nutrition for yeast while triggering more inflammation. The self-perpetuating cycle explains why fungal acne often persists without intervention.
Your skin barrier function plays a crucial role in this process. A healthy barrier maintains proper pH levels, regulates moisture content, and supports beneficial microbiome diversity. When humidity, sweating, and occlusive products compromise barrier integrity, the skin environment shifts toward conditions favoring yeast dominance over balanced microbial populations.
Distinguishing Fungal Acne From Other Skin Conditions
| Feature | Fungal Acne | Bacterial Acne | Heat Rash |
|---|---|---|---|
| Appearance | Uniform small bumps | Varied sizes, comedones | Tiny red bumps, clusters |
| Itchiness | Often itchy | Rarely itchy | Very itchy, prickly |
| Distribution | Forehead, chest, back | Face, jawline, back | Skin folds, covered areas |
| Response to acne treatment | Worsens or no change | Typically improves | No response |
| Trigger pattern | Humidity, sweat | Hormones, stress | Trapped sweat, heat |
Several conditions present similarly to fungal acne, making visual identification challenging. Bacterial acne produces lesions of varying sizes, including blackheads, whiteheads, papules, and cysts. The distribution pattern differs too, with bacterial acne favoring the face, particularly the jawline and chin, while fungal acne commonly affects the chest, shoulders, and upper back.
Heat rash develops when sweat ducts become blocked, creating tiny fluid-filled bumps that feel prickly and intensely itchy. Unlike fungal acne, heat rash resolves quickly once you cool down and typically appears in areas where clothing traps sweat, such as under breasts or in skin folds.
The treatment response pattern provides the clearest distinction. If your bumps worsen or remain unchanged after four weeks of consistent acne treatment, fungal acne becomes more likely. Traditional acne medications containing antibiotics and ingredients that can worsen fungal acne by eliminating bacteria that normally compete with yeast for resources.
Environmental and Lifestyle Modifications That Help
Creating an environment less favorable to yeast growth requires understanding how daily choices affect skin conditions. Choosing clothing fabrics strategically makes substantial difference in humid climates. Natural fibers like cotton, linen, and bamboo allow air circulation and moisture wicking better than synthetic materials. Loose-fitting garments prevent the occlusive microenvironment that traps sweat against skin.
Timing your cleansing routine around sweat exposure matters significantly. Showering within 30 minutes after sweating removes the sweat-sebum mixture before yeast populations can multiply substantially. If immediate showering isn't possible, changing into dry, breathable clothing and using a clean towel to pat away surface moisture provides temporary benefit until proper cleansing.
Managing indoor humidity levels helps reduce overall exposure to moisture. Using dehumidifiers in bedrooms maintains air moisture below the 60 percent threshold where yeast thrives. This intervention proves particularly valuable during sleep, when you spend 6–8 consecutive hours in one environment.
Adjusting your skincare approach prevents inadvertent yeast feeding. Avoiding products containing oils, esters, fatty acids, and polysorbates eliminates ingredients that malassezia metabolizes. Lightweight, gel-based formulations provide hydration without creating occlusive barriers. Maintaining skin pH between 4.5–5.5 through pH-balanced cleansers creates conditions less favorable to yeast overgrowth while supporting beneficial bacteria.
The Skin Barrier Connection
Your skin barrier serves as the first defense against microbial imbalances, making its integrity crucial for managing fungal acne. The barrier consists of corneocytes embedded in lipid layers, functioning like bricks and mortar to regulate moisture, maintain pH, and support healthy microbiome diversity.
When high humidity combines with aggressive cleansing or harsh products, barrier lipids become depleted. This depletion allows increased transepidermal water loss while simultaneously making skin more permeable to irritants. The compromised barrier loses its ability to maintain the slightly acidic pH that supports beneficial bacteria, allowing yeast populations to expand unchecked.
Barrier repair requires gentle cleansing that removes sweat and excess sebum without stripping protective lipids. Over-washing, even with appropriate cleansers, depletes the lipid layer faster than your skin can rebuild it. In humid climates, cleansing twice daily typically provides adequate hygiene without compromising barrier function, though individual needs vary based on activity levels.
Supporting barrier recovery involves providing ceramides, cholesterol, and fatty acids in ratios that mimic natural skin lipids. However, choosing barrier repair products requires care with fungal acne, as some lipid formulations feed yeast. Products specifically formulated to avoid malassezia-feeding ingredients while supporting barrier function help restore skin integrity without worsening overgrowth.
Dietary and Internal Factors
While external moisture and heat create favorable surface conditions for yeast, internal factors influence how readily your skin develops fungal acne. Diets high in simple carbohydrates and sugars may increase sebum production and alter sebum composition, potentially making it more favorable for yeast metabolism. This connection appears stronger in individuals with insulin resistance or metabolic concerns.
Systemic inflammation from poor sleep, chronic stress, or inflammatory dietary patterns affects skin immune function. Elevated cortisol from ongoing stress can increase oil production while simultaneously suppressing local immune responses that normally keep yeast populations in check. Sleep deprivation similarly impairs skin barrier repair and immune surveillance.
Gut microbiome health influences skin microbiome balance through complex immune and metabolic pathways. Disrupted gut bacteria from antibiotic use, poor fiber intake, or digestive conditions may correlate with skin dysbiosis, including yeast overgrowth. While research continues exploring these connections, the gut-skin axis appears relevant to fungal acne susceptibility.
Hydration status affects sebum consistency and skin barrier function. Dehydration leads to more viscous sebum that flows less freely from follicles, creating blockages where yeast can proliferate. Adequate water intake supports sebum flow and barrier hydration, creating less stagnant follicular environments.
When Professional Evaluation Becomes Necessary
Several situations warrant dermatological consultation rather than continued self-management. If your bumps persist despite four weeks of appropriate environmental modifications and gentle skincare, professional evaluation helps confirm whether you're truly dealing with fungal acne or another condition requiring different intervention.
Widespread involvement covering large areas of your chest, back, or face suggests significant microbiome imbalance that may benefit from targeted treatment. Similarly, severe itching that interferes with sleep or daily activities indicates inflammation levels requiring professional attention.
Signs of secondary infection, including increasing pain, warmth, swelling, or pustule formation with yellow or green discharge, require prompt evaluation. These symptoms suggest bacterial infection has developed alongside or instead of fungal overgrowth, necessitating different treatment approaches.
Recurring episodes despite successful previous management may indicate underlying factors like compromised immunity, hormonal imbalances, or medication effects that deserve investigation. Conditions like diabetes, immune suppression, or certain medications can predispose you to recurrent fungal skin issues.
A dermatologist can perform definitive diagnosis through clinical examination or skin sampling. They can also assess whether you have both fungal and bacterial components, a common scenario that requires addressing both organisms. Professional guidance becomes particularly valuable when initial approaches haven't provided expected improvement.
Prevention Strategies for Long-Term Management
| Strategy | How It Helps | Implementation |
|---|---|---|
| Quick post-sweat cleansing | Removes yeast food source | Shower within 30 minutes of sweating |
| Breathable fabrics | Allows moisture evaporation | Choose cotton, linen, bamboo |
| Clean clothing daily | Prevents yeast reintroduction | Change shirts, especially after sweating |
| pH-balanced products | Maintains protective acid mantle | Use cleansers around pH 5 |
| Barrier support | Strengthens microbial defense | Apply appropriate barrier repair |
Long-term fungal acne management in humid climates requires consistent attention to factors that influence yeast proliferation. Prevention focuses on maintaining conditions unfavorable to overgrowth rather than attempting to eliminate yeast completely, which isn't possible since malassezia is a normal skin resident.
Establishing reliable post-activity hygiene routines prevents yeast from exploiting the sweat-sebum environment. This doesn't require obsessive cleansing but rather timely removal of the moisture and nutrients that fuel rapid multiplication. Even rinsing with water and changing clothes provides benefit when full showering isn't immediately possible.
Regular laundering of items that contact affected areas prevents reintroduction of yeast populations. Towels, pillowcases, and clothing that touch your chest, back, or face should be washed after each use rather than reused over multiple days. Hot water washing and complete drying further reduce yeast survival on fabrics.
Maintaining skin barrier integrity through appropriate product selection and avoiding over-treatment supports your skin's natural ability to regulate its microbiome. A healthy barrier creates an environment where beneficial bacteria can compete effectively with yeast, preventing any single organism from dominating.
Awareness of your individual trigger patterns allows proactive adjustment during high-risk periods. If you notice flares consistently during specific months, activities, or situations, you can intensify preventive measures during those times rather than maintaining maximum vigilance year-round.
Understanding Internal Triggers: Clear Ritual's Perspective
Fungal acne develops from multiple interacting factors including environmental humidity, sebum production, barrier function, microbiome balance, stress responses, sleep quality, and metabolic health. While external modifications like breathable clothing and timely cleansing address surface conditions, they may not resolve underlying susceptibility patterns that make some individuals more prone to yeast overgrowth than others.
At Clear Ritual, we combine the best of three worlds - Ayurveda, modern dermatology, and advanced skin science - to understand individual triggers through a structured Clear Ritual Skin Test assessment. This approach recognizes that two people in identical humid climates may experience vastly different fungal acne patterns based on their unique internal environments, stress responses, dietary patterns, and skin barrier characteristics.
Understanding your specific trigger combination helps explain why certain preventive measures work better for you than others and why your fungal acne may behave differently than another person's despite similar external conditions. This personalized understanding supports more stable long-term skin balance rather than temporary symptom suppression.
Frequently Asked Questions
Can fungal acne spread to other people?
Fungal acne itself doesn't spread person-to-person because everyone already has malassezia yeast on their skin naturally. However, factors that trigger overgrowth, like sharing sweaty clothing or towels, could transfer larger yeast populations. The condition develops based on individual susceptibility and environmental conditions rather than contagion.
Why does my fungal acne get worse when I use acne treatments?
Traditional acne treatments containing benzoyl peroxide or antibiotics target bacteria, not yeast. Antibiotics can actually worsen fungal acne by killing beneficial bacteria that normally compete with yeast for resources. Additionally, many acne products contain oils or ingredients that feed malassezia, directly supporting the organisms causing your bumps.
How long does it take for fungal acne to clear?
The timeline varies significantly based on severity, environmental factors, and how consistently you modify triggers. With appropriate changes to reduce yeast-favorable conditions, many people notice improvement within 2–4 weeks. However, complete clearance may require 6–8 weeks, and ongoing prevention remains necessary in humid climates to prevent recurrence.
Can diet changes help with fungal acne?
Diet influences fungal acne indirectly by affecting sebum production, inflammation levels, and overall skin health. Reducing high-glycemic foods may decrease sebum output, while anti-inflammatory eating patterns support skin barrier function. However, dietary changes alone rarely resolve fungal acne without addressing external moisture and occlusion factors.
Is fungal acne only a problem in tropical countries?
While more common in tropical and humid climates, fungal acne can develop anywhere conditions favor yeast growth. Athletes who sweat frequently, people who wear occlusive clothing for long periods, or individuals with compromised immunity can develop fungal acne even in temperate climates. Summer months increase risk regardless of geographic location.
Does fungal acne leave scars?
Fungal acne typically causes less scarring than bacterial acne because the inflammation remains more superficial. However, picking or scratching the itchy bumps can lead to post-inflammatory hyperpigmentation or acne scars. Severe cases with deep inflammation may occasionally leave marks, making early intervention important.
Can I wear makeup if I have fungal acne?
You can wear makeup, but product selection matters significantly. Avoid foundations, primers, and creams containing oils, fatty acids, or esters that feed malassezia yeast. Mineral-based, powder formulations generally prove safer than cream or liquid products. Always remove makeup thoroughly and promptly after wear to prevent prolonged follicle occlusion.
Why does fungal acne itch when regular acne doesn't?
The itching occurs because your immune system recognizes malassezia overgrowth as abnormal and triggers inflammatory responses that include histamine release. Yeast organisms also produce metabolic byproducts that irritate follicle linings. Bacterial acne involves different inflammatory pathways that typically don't activate the same itch-producing mechanisms.
Editorial Standards
Clear Ritual has Strict sourcing guidelines to ensure our content is accurate and current. We rely on peer-reviewed studies, academic research institutions, and medical associations. We strive to use primary sources and refrain from using tertiary references. See a mistake? Learn More about our Editorial Standards.
Related Articles
Antibiotics and Fungal Acne: Understanding the Link
Published June 6, 2026

Do You Have Fungal Acne? Here's How It's Different From Bacterial Breakouts
Published May 26, 2026

Fungal Acne: Causes, Symptoms, Treatment & Prevention Tips
Published May 26, 2026

Fungal Acne on Back and Chest
Published May 26, 2026