Forehead Acne vs Fungal Acne: Differences in Causes and Treatment
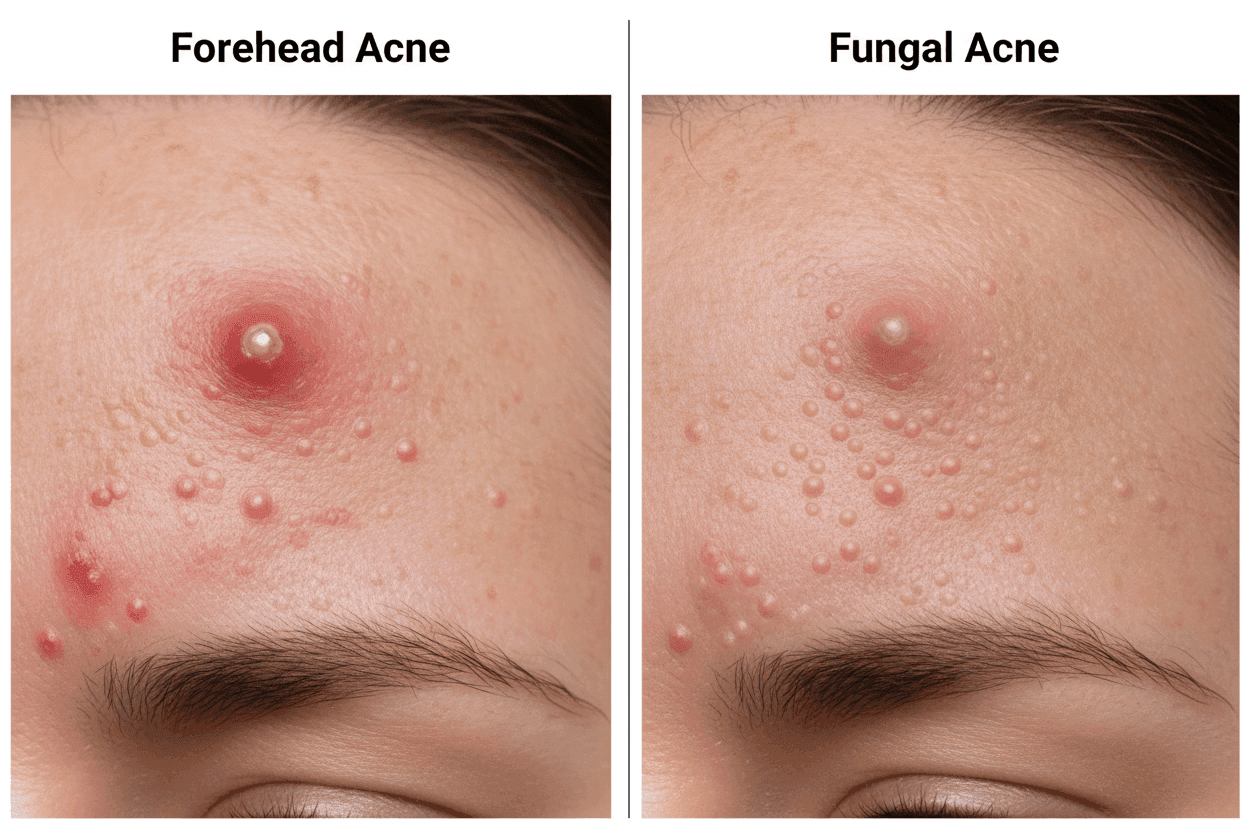
Forehead acne (bacterial acne) is caused by Cutibacterium acnes bacteria multiplying inside a clogged, oil-blocked pore. Fungal acne — medically called Malassezia folliculitis or Pityrosporum folliculitis — is caused by yeast overgrowth inside the hair follicle and does not respond to standard acne products.
The single fastest way to tell them apart: fungal acne itches; bacterial forehead acne usually does not.
Three other quick signs:
- Fungal acne bumps are all the same small size; bacterial acne bumps vary
- Fungal acne appears in even clusters across the forehead, chest, or back; bacterial acne clusters unevenly
- Standard acne serums often make fungal acne worse instead of better
Understanding which type you have determines the treatment approach that will actually work.
Forehead acne typically results from excess sebum and bacteria clogging pores, appearing as whiteheads, blackheads, or inflamed pustules. Fungal acne, caused by yeast overgrowth, shows up as uniform small bumps that are itchy and don't respond to standard acne treatments.
Key Takeaways
- Forehead acne involves bacterial infection in clogged pores, while fungal acne is caused by yeast (Malassezia) overgrowth
- Bacterial acne appears as varied-sized pimples; fungal acne presents as uniform, itchy bumps
- Traditional acne treatments may worsen fungal acne
- Location, appearance, and accompanying symptoms help differentiate between the two
- Each condition requires a different treatment approach
What Forehead Acne Really Is
Forehead acne develops when hair follicles become blocked with a combination of dead skin cells, sebum, and bacteria. The forehead sits within the T-zone, an area with higher sebaceous gland density that produces more oil throughout the day.
When oil mixes with skin cells that haven't shed properly, it creates an environment where Cutibacterium acnes bacteria thrive.
The forehead is particularly vulnerable to external triggers:
- Hair products containing silicones or oils migrating onto the skin
- Sweat accumulation under hats or headbands
- Repeated touching of the forehead transferring oil and bacteria
- Pollution and debris mixing with sebum
Inside a blocked follicle, oxygen levels drop. C. acnes bacteria multiply rapidly in this low-oxygen environment, triggering inflammation, redness, swelling, and painful pimples.
Understanding Fungal Acne
Fungal acne isn't technically acne at all.
The medical term is Malassezia folliculitis or Pityrosporum folliculitis. Instead of bacteria, this condition involves an overgrowth of yeast that naturally lives on everyone's skin.
Malassezia feeds on fatty acids found in sebum. When conditions favor yeast growth, it multiplies inside hair follicles and triggers inflammation that appears as small, uniform bumps.
Unlike bacterial acne, fungal acne frequently appears on:
- Forehead
- Chest
- Shoulders
- Upper back
These are areas with high oil production and more heat/moisture retention.
How to Tell Them Apart
| Feature | Forehead Acne | Fungal Acne |
|---|---|---|
| Appearance | Mixed sizes, whiteheads, blackheads, cysts | Uniform small bumps |
| Itchiness | Minimal to none | Often itchy |
| Distribution | Uneven clustering | Even pattern |
| Response to acne treatment | Usually improves | Often worsens |
| Timing | Gradual development | Can appear suddenly |
The itching factor is particularly important. Bacterial acne may feel tender or painful, but fungal acne often produces persistent itchiness that worsens with heat or sweating.
How to Tell If Your Forehead Bumps Are Fungal or Bacterial: A Step-by-Step Check
Step 1: Look at the Size and Shape
Bacterial forehead acne shows variation:
- Some bumps are large
- Some are small
- Some contain pus or blackheads
- Some are inflamed
Fungal acne bumps are usually:
- Uniform in size
- Roughly 1–2 mm
- Dome-shaped
- Without visible blackheads or whiteheads
If every bump looks nearly identical, suspect fungal acne first.
Step 2: Check for Itching
Bacterial acne is usually sore or tender when touched.
Fungal acne often:
- Itches even without touching
- Gets worse after sweating
- Becomes itchier in humid weather
- Flares at night
This happens because yeast triggers histamine release in the skin.
Step 3: Map the Distribution
Bacterial acne typically clusters in isolated zones such as:
- Hairline
- Temples
- Forehead center
Fungal acne spreads more evenly across:
- Forehead
- Chest
- Upper back
- Shoulders
Step 4: Review Recent Triggers
Ask yourself:
- Have you recently taken antibiotics?
- Have you been sweating heavily?
- Did you switch to a richer moisturizer or facial oil?
- Are you living in a humid climate?
- Have stress levels increased recently?
These are major fungal acne triggers because they favor yeast overgrowth.
Step 5: Run a Two-Week Treatment Test
Use a salicylic acid or benzoyl peroxide treatment consistently for two weeks.
If it improves:
You’re likely dealing with bacterial acne.
If it worsens or stays identical:
Fungal acne becomes more likely.
At that point, switching to antifungal treatment is recommended.
This guide is not a medical diagnosis. If symptoms worsen or persist beyond six weeks, consult a dermatologist.
What Triggers Forehead Acne
Forehead acne is commonly triggered by:
- Excess sebum production
- Hormonal fluctuations
- Stress and elevated cortisol
- Sleep deprivation
- High glycemic diets
- Pollution buildup
- Hair products clogging pores
- Overwashing and barrier damage
Sebum-heavy skin creates the perfect environment for clogged pores and bacterial overgrowth.
What Triggers Fungal Acne
Fungal acne thrives in warm, moist, oily environments.
Common triggers include:
- Humid climates
- Sweaty workout clothing
- Antibiotic use
- Heavy oils and rich moisturizers
- Occlusive skincare products
- Immune system imbalance
- Stress-related microbiome disruption
Antibiotics are a particularly common trigger because they remove bacterial competition, allowing yeast populations to grow rapidly.
What Research Says About Fungal Acne and Forehead Breakouts
Research increasingly shows that fungal acne is commonly misdiagnosed as regular acne.
Studies have found:
- Antibiotics can worsen Malassezia overgrowth
- Lipid-rich skincare products can feed fungal acne
- Skin barrier disruption worsens both bacterial and fungal acne
- Salicylic acid effectively reduces inflammatory acne lesions
- Sebum composition influences susceptibility to both conditions
Treatment Approaches for Forehead Acne
1. Gentle Cleansing
Use a balanced cleanser twice daily to remove excess oil without damaging the skin barrier.
Avoid:
- Harsh scrubs
- Over-cleansing
- Alcohol-heavy cleansers
2. Salicylic Acid
Salicylic acid works inside the pore to dissolve dead skin buildup and reduce inflammation.
Benefits include:
- Oil control
- Exfoliation
- Reduced congestion
- Fewer clogged pores
3. Benzoyl Peroxide
Benzoyl peroxide introduces oxygen into pores, killing acne-causing bacteria.
Start with lower strengths to reduce irritation.
4. Niacinamide
Niacinamide helps:
- Reduce inflammation
- Strengthen the skin barrier
- Control sebum production
- Calm redness
5. Retinoids
Retinoids increase skin cell turnover and help prevent clogged pores.
They are particularly effective for:
- Comedonal acne
- Texture irregularities
- Post-acne marks
Treatment Approaches for Fungal Acne
1. Zinc Pyrithione
Commonly found in dandruff shampoos, zinc pyrithione has antifungal properties that help reduce Malassezia overgrowth.
2. Sulfur
Sulfur acts as:
- Antifungal
- Anti-inflammatory
- Mild exfoliant
It is often gentler than stronger antifungal medications.
3. Avoid Heavy Oils
Avoid products containing:
- Olive oil
- Coconut oil
- Argan oil
- Fatty acid-rich formulations
Switch to lightweight, gel-based moisturizers instead.
4. Keep Skin Cool and Dry
Helpful strategies include:
- Showering after sweating
- Wearing breathable fabrics
- Avoiding prolonged sweat exposure
- Changing workout clothes immediately
5. Prescription Antifungals
Persistent fungal acne may require prescription treatments such as:
- Ketoconazole
- Fluconazole
- Itraconazole
Consult a dermatologist for severe or resistant cases.
Fungal Acne–Safe vs. Fungal Acne–Feeding Ingredients
Ingredients That May Feed Malassezia
| Ingredient Category | Common Examples | Why It's a Problem |
|---|---|---|
| Fatty acids | Oleic acid, lauric acid | Feed yeast directly |
| Plant oils | Olive oil, almond oil | High fatty acid content |
| Esters | Isopropyl myristate | Break down into fatty acids |
| Ferments | Yeast extracts | May worsen imbalance |
| Polysorbates | Polysorbate 20/60/80 | Can feed yeast |
Ingredients Generally Considered Fungal-Acne Safe
| Ingredient | Benefit |
|---|---|
| Squalane | Lightweight hydration |
| Niacinamide | Anti-inflammatory |
| Hyaluronic acid | Hydration without oils |
| Zinc pyrithione | Antifungal |
| Ketoconazole | Prescription antifungal |
| Sulfur | Antifungal + keratolytic |
| Salicylic acid | Oil-soluble exfoliation |
| Azelaic acid | Anti-inflammatory |
| Glycerin | Humectant hydration |
Forehead Acne vs. Fungal Acne Treatment Comparison
| Treatment Factor | Forehead Acne | Fungal Acne |
|---|---|---|
| Main trigger | Bacteria + clogged pores | Yeast overgrowth |
| First-line treatment | Salicylic acid, benzoyl peroxide | Zinc pyrithione, ketoconazole |
| Antibiotics | Helpful | Often worsen condition |
| Heavy oils | Sometimes tolerated | Usually worsen condition |
| Improvement timeline | 4–8 weeks | 2–6 weeks |
| Risk of recurrence | Moderate | High in humid environments |
When You May Have Both Conditions
It is possible to have bacterial acne and fungal acne simultaneously.
Signs include:
- Traditional pimples plus itchy uniform bumps
- Acne that partially improves but never fully clears
- Breakouts spreading across forehead, chest, and back
In these cases, treatment must address both bacteria and yeast carefully.
When Standard Treatments Don’t Work
If your forehead bumps:
- Persist beyond six weeks
- Worsen with acne products
- Spread rapidly
- Become extremely itchy
- Appear across chest and back
…fungal acne becomes increasingly likely.
Professional evaluation may be necessary.
When to See a Dermatologist
See a dermatologist if:
- Symptoms persist despite treatment
- Breakouts are painful or spreading
- You are unsure whether it is fungal or bacterial
- You have diabetes or immune-related conditions
- Over-the-counter products fail repeatedly
A dermatologist may perform:
- KOH testing
- Skin scraping
- Microscopic examination
These tests can confirm fungal involvement quickly.
The Role of Skin Barrier Health
Both conditions worsen when the skin barrier becomes damaged.
Barrier disruption leads to:
- Increased inflammation
- More oil production
- Higher transepidermal water loss
- Greater microbial imbalance
Supporting barrier health involves:
- Gentle cleansing
- Avoiding over-exfoliation
- Maintaining hydration
- Using barrier-supportive ingredients like ceramides and niacinamide
Lifestyle Factors That Matter
Several lifestyle factors influence both acne types:
Sleep
Poor sleep increases cortisol and inflammation.
Diet
High glycemic foods may worsen oil production and inflammation.
Stress
Stress disrupts:
- Hormones
- Immune function
- Skin microbiome balance
Hydration
Dehydration thickens sebum and may worsen clogged pores.
Frequently Asked Questions
Can fungal acne turn into regular acne?
No. They are separate conditions, though they can occur together.
Why does my forehead acne worsen with acne products?
If the condition is fungal, antibacterial products may worsen yeast imbalance.
How long does fungal acne take to clear?
Most people notice improvement within 2–4 weeks, with fuller clearing in 6–8 weeks.
Can I use the same moisturizer for both?
Lightweight, gel-based, oil-free moisturizers are usually safest for both conditions.
Does diet affect fungal acne?
Diet may indirectly affect fungal acne through sebum production and inflammation.
Why does fungal acne itch?
Yeast triggers histamine-related immune responses that activate itch receptors.
Can stress worsen both conditions?
Yes. Stress affects hormones, inflammation, immune function, and sebum production.
Should I see a dermatologist for small forehead bumps?
If bumps persist beyond 4–6 weeks or worsen despite treatment, professional evaluation is recommended.
What This Means for You
Most people with persistent forehead bumps are unknowingly treating the wrong condition.
Once you correctly identify whether your breakout is:
- Bacterial
- Fungal
- Or both
…the right treatment usually works within four to six weeks.
What to Do Next
- Run the five-step assessment before buying new products
- Check moisturizer ingredients carefully
- Use salicylic acid and niacinamide if bacterial acne is likely
- Remove heavy oils and use antifungal washes if fungal acne is suspected
- Consult a dermatologist if improvement stalls after six weeks
If you've cycled through multiple products without lasting improvement, the missing piece is often identifying the underlying trigger — whether hormonal, microbial, barrier-related, or lifestyle-driven.
Editorial Standards
Clear Ritual has Strict sourcing guidelines to ensure our content is accurate and current. We rely on peer-reviewed studies, academic research institutions, and medical associations. We strive to use primary sources and refrain from using tertiary references. See a mistake? Learn More about our Editorial Standards.



