Fungal Acne: Causes, Symptoms, Treatment & Prevention Tips

Fungal acne, also known as Malassezia folliculitis, is a skin infection caused by the excessive yeast production in the hair follicles. It appears as small, bumpy, red acne in clusters on the face and different parts of the body, such as the chest, back, and shoulders. Some of them also have a pus-filled appearance, which is a white-yellow fluid. Fungal acne is usually itchy and has a burning sensation. It can get worse in humid, sweaty conditions. To treat your fungal acne, your doctor may prescribe oral and topical treatment, which you need to follow to manage the breakouts.
If you have tried a traditional acne treatment and still see the bumps on your forehead and other parts of the body, you are likely dealing with fungal acne. Regular treatment, such as using active skincare products, does not work to manage or treat the condition. It always requires a professional consultation. This article covers what is fungal acne, its symptoms, causes, in-office treatment and the differences between fungal acne and regular acne so you can treat it effectively. Keep reading to know more.
What is Fungal Acne?
Fungal acne, also known as Malassezia folliculitis and Pityrosporum folliculitis, is caused by the growth of Malassezia fungus in the skin follicles. This acne is different from regular acne, which is triggered by clogged pores, dead skin cells, and bacteria. Fungal acne is generally itchy, small, bumpy and often red in colour. They may or may not be pus-filled. They commonly occur on the forehead and upper body, such as the chest, shoulders, neck, and back.
Symptoms of Fungal Acne
While fungal acne can look similar to regular acne, it has major differences in terms of symptoms. The following are some fungal acne symptoms you need to know:
- They are red or white, bumpy acne
- They are itchy, painful, or have a burning sensation
- They appear in clusters and give a prickly sensation
- They appear on the forehead, chest, chin, neck, upper arms, and shoulders.
- They often occur in groups rather than individually
Causes of Fungal Acne
We all have Malassezia fungus on our skin. The problem starts when it enters the damaged hair follicles. Here are some other causes of fungal acne that can worsen the breakouts.
- Shaving or waxing skin hair
- Touching your skin with dirty hands
- Excess sweat and humidity
- Leaving sweat on your skin after exercise
- Showering with extremely hot water
- Workout a lot regularly without showering immediately after it
- Using a greasy cosmetic
- Wearing fitted clothes (for body fungal acne)
People who live in humid weather, especially in cities like Mumbai or other coastal cities, are more prone to getting fungal acne.
Diagnosis of Fungal Acne
Unlike traditional acne, fungal acne is a skin infection that needs professional treatment. An examination will help the doctor understand whether you have a fungal skin infection or a certain type of acne. The process starts with a Wood’s lamp or a small black light to examine your face and detect fungal bacteria.
Malassezia yeast glows under the light. Your doctor may gently scrape the areas with acne once they find fungus. Then, they keep the scraped skin cells under the microscope to identify the yeast causing fungal acne.
Differences Between Fungal Acne and Comedonal Acne
It is quite common for people to confuse comedonal acne with fungal acne, as they look somewhat identical. So, if you are wondering whether there is some way to spot the difference between them. Then yes, here are a few key differences that can help you understand the type of acne you have:
| Fungal Acne | Comedonal Acne |
|---|---|
| Caused by yeast overgrowth | Caused by clogged pores. |
| Often itchy. | Usually not itchy. |
| Red or inflamed bumps. | Skin-colored bumps. |
| Needs antifungal treatment. | Responds to exfoliation. |
Comedonal acne usually feels rough when you touch it and is painless. Fungal acne can often feel itchy or irritating.
Treatment of Fungal Acne
Fungal acne treatment involves topical antifungal medication and oral medications. Your doctor will examine your breakouts to understand which one your skin requires. Listed below are the different medications prescribed to treat fungal acne.
Oral Medications include:
- Fluconazole
- Itraconazole
Topical Medications include:
- Ketoconazole
- Econazole
- Clotrimazole
- Selenium shampoo (for body)
Applying these Malassezia folliculitis medicines for weeks to months can significantly reduce the symptoms of fungal acne. Oral medication is generally used to treat fungal acne if the fungus has penetrated the hair follicles.
What Are the Prevention Tips for Fungal Acne?
Knowing the prevention tips for Malassezia folliculitis is as important as treating the condition. It can help you avoid habits that can cause fungal acne from recurring. Given below are some tips to prevent fungal acne.
- Immediately change your clothes after working out
- Be cautious while shaving, waxing, or plucking hair
- Frequently clean your bathrobe and towels
- Wear loose clothes, especially in hot weather
- Avoid overwashing your face
- Use a non-comedogenic moisturiser
- Reducing high-sugar, high-carb intake and dairy products
Differences Between Fungal Acne and Regular Acne
Fungal acne and regular acne have similar appearances but major differences in symptoms, causes, and treatment. The table below will help you understand the major differences between them so you can treat them effectively.
| Fungal Acne | Regular Acne |
|---|---|
| It is caused by the overgrowth of fungus (Malassezia) in the hair pores | It is caused by excess oil production, dead skin cells, and bacteria penetrating the pores |
| They are small, bumpy breakouts of almost the same size, appearing in a cluster form | They are bumpy, inflamed acne and can be in various forms like blackheads, whiteheads, papules, and pustules |
| The fungal acne has a rough texture like a tiny sandpaper bump, but is usually red in colour | The regular acne can be bumpy, inflamed, rough, or pus-filled |
| They appear on the chest, neck, shoulders, back and forehead areas | They appear on the face, generally on the T-zone, chest, and back |
| It requires professional help and can’t be managed with regular acne treatment | It can be managed with active ingredients like salicylic acid, benzoyl peroxide, and retinoids |
When to See a Doctor for Fungal Acne?
Since Malassezia acne and regular acne look similar, people are likely to follow regular acne treatments for fungal acne, not realising they are different. If the acne doesn’t disappear or is not managed with regular acne treatment, you must consult your doctor immediately. They will examine your breakouts to determine whether you have a Malassezia folliculitis or traditional acne.
Your doctor will recommend some oral and topical medication which needs to be followed for weeks and months. Once your fungal acne disappears or starts to fade, ensure to take the prevention tips to reduce the risk of recurrence.
Who Can Be Infected By Fungal Acne?
Fungal acne can affect people of all ages, but it is common in young adults, especially people with oily skin. The following are some conditions that cause fungal acne:
- Spending too much time in a humid climate
- Using heavyweight skincare products
- Ignoring your health and sticking to poor dietary habits
- Infection with other fungal skin conditions, such as seborrheic dermatitis
Are There Any Side Effects of Fungal Acne?
Oral treatment may have certain side effects such as diarrhoea, nausea, vomiting, or stomachache. In rare cases, oral medication also causes liver damage symptoms. These side effects are the reasons why your doctor may switch to topical treatment or prescribe them even before recommending oral treatment. This helps the doctor understand which kind of medication suits your body. If your doctor has already prescribed oral medication and you are suffering from these side effects, consult your doctor immediately.
People with oily skin often get fungal acne. If you fall into the same category, your doctor may recommend long-term medical treatment or photodynamic therapy. Using this treatment, the doctor kills the fungal bacteria existing on your skin. Photodynamic therapy is taken into consideration, especially when other anti-fungal medications aren’t working.
Clear Ritual’s Perspective on Treating Fungal Acne
Fungal acne isn’t a surface-level issue that shows up on your skin and can go away on its own. There are many lifestyle factors and habits that trigger fungal acne breakouts.
Anything that causes imbalance in your skin, right from sleep deprivation, poor sleep cycle, stress, excessive sweating, damaged skin barrier, or skincare that doesn’t suit your skin, can unknowingly contribute to the fungal acne and irritation.
At Clear Ritual, we believe that your focus shouldn’t be just on reducing the existing fungal acne or bumps on the skin temporarily. The idea is to create a sustainable approach and lifestyle that helps you stop the actions that trigger those conditions. Understanding symptoms and treatments is a later part.
If you identify the root cause correctly and manage fungal acne in the right way, it becomes much easier to manage. And achieving healthy skin becomes far more achievable.
Frequently Asked Questions
How to get rid of fungal acne?
You can get rid of fungal acne by taking the anti-fungal medication and using the fungal acne-safe skincare products. Your doctor will recommend and prescribe some of them when you seek professional help.
What are the home remedies for fungal acne?
You can use non-comedogenic skincare products and a sulfate-based cleanser to fix fungal acne. However, though it can help you manage the Malassezia yeast acne, it won’t treat it at its core. It's better to consult your doctor when you get fungal acne than to rely on home remedies.
How can I tell whether my acne is fungal?
When you treat your fungal acne using the traditional treatment and the acne doesn’t respond to it, you are likely to have fungal acne. You can try some management and prevention tips for Malassezia acne, but for the proper treatment, it requires professional help.
Why am I suddenly experiencing fungal acne?
While Malassezia yeast is present on our skin all the time, the fungal acne occurs when the yeast enters the hair follicles due to a hot climate and excessive sweating. For instance, if you do not shower immediately after working out, sweat may cause fungal acne.
Which foods can worsen fungal acne?
High-carb foods and dairy products are the main foods that worsen fungal acne. This includes white bread, white rice, pasta, milk, cheese, alcohol, pizza, chocolates, and any sugary products.
What to avoid if you have fungal acne?
When you have fungal acne, what you need to do initially is avoid doing things that can worsen your condition, such as waxing or shaving the affected area, not having a bath, or exposing yourself to high humidity.
Reference Links
Editorial Standards
Clear Ritual has Strict sourcing guidelines to ensure our content is accurate and current. We rely on peer-reviewed studies, academic research institutions, and medical associations. We strive to use primary sources and refrain from using tertiary references. See a mistake? Learn More about our Editorial Standards.
Related Articles
Antibiotics and Fungal Acne: Understanding the Link
Published June 6, 2026

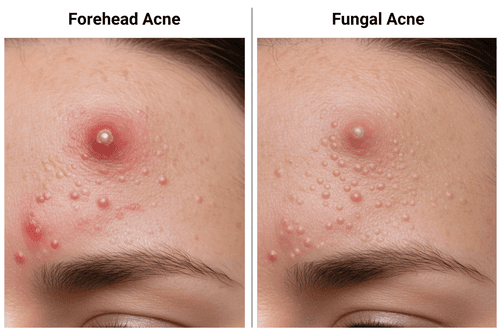
Forehead Acne vs Fungal Acne: Differences in Causes and Treatment
Published May 26, 2026
Do You Have Fungal Acne? Here's How It's Different From Bacterial Breakouts
Published May 26, 2026

Fungal Acne in Humid and Tropical Weather
Published June 6, 2026


