What Are Those Small Bumps on Your Face? It Might Not Be Acne

Let’s Be Honest: Not Every Bump Is a Breakout
You’ve tried the face wash, the salicylic acid, the spot treatment. And yet… those tiny bumps on your cheeks, forehead, or chin just won’t budge.
That’s probably because they’re not acne.
They may look like whiteheads or closed comedones, but the underlying cause - and therefore the treatment - is very different.
Misdiagnosing these bumps often leads to:
- Worsening texture
- Redness and irritation
- Wasted weeks on the wrong routine
Let’s break down what else these mystery bumps could be - and what to do instead of nuking them with harsh actives.
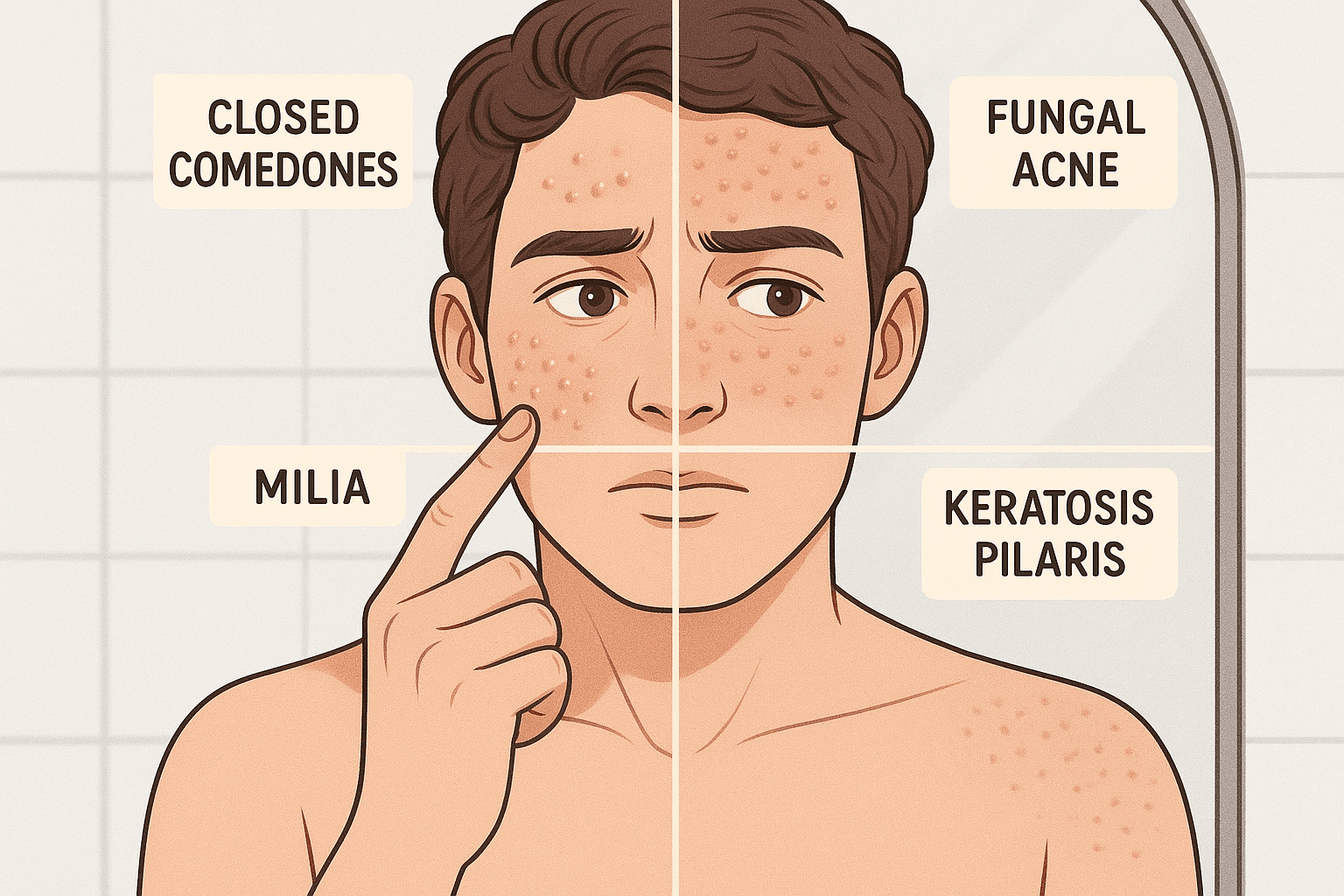
Acne Lookalikes: What Could Those Bumps Actually Be?
| Condition | Description | Common Location | Main Cause |
|---|---|---|---|
| Closed Comedones | Small, skin-colored bumps that feel rough | Cheeks, forehead | Clogged pores with dead skin and sebum |
| Fungal Acne (Malassezia Folliculitis) | Itchy, uniform bumps, sometimes red | Forehead, hairline, chest | Yeast overgrowth in hair follicles |
| Milia | Hard, tiny white bumps under the skin | Around eyes, cheeks | Trapped keratin under the skin |
1. Closed Comedones (The Usual Suspect)
These are technically still acne, but non-inflammatory.
They feel like texture - not red, not painful, just bumpy.
What causes them?
- Dead skin cells not shedding properly
- Excess sebum
- Occlusive skincare or makeup
- Poor cleansing habits
How to treat:
- Introduce chemical exfoliation (salicylic or glycolic acid)
- Use non-comedogenic moisturisers
- Avoid pore-clogging ingredients (look out for heavy oils, silicones)
This is the most responsive to classic acne routines - but if your bumps don’t go away, it may be one of the next three.
2. Fungal Acne (Malassezia Folliculitis)
Despite the name, this isn’t true acne. It’s a yeast-based infection of the hair follicles caused by an overgrowth of Malassezia - a fungus that naturally lives on our skin.
How to identify it:
- All the bumps look similar in size
- They often itch
- They show up in clusters (especially on forehead, back, or chest)
- Traditional acne treatments make it worse
What causes fungal acne?
- High humidity and sweat
- Wearing occlusive makeup or helmets for long periods
- Overuse of antibiotics or steroids
- Imbalance in skin’s microbiome
How to treat fungal acne:
- Use antifungal ingredients like ketoconazole, zinc pyrithione, or selenium sulfide
- Switch to fungal-safe skincare (no esters or oils that feed Malassezia)
- Keep skin dry and breathable - avoid over-moisturising
Chemical exfoliants like salicylic acid won’t help here - and might aggravate the condition.
3. Milia (Keratin Cysts, Not Acne)
Milia are those small, white, hard bumps that often appear around the eyes or cheeks.
They’re not filled with oil, pus, or bacteria - they’re made of trapped keratin.
How to spot milia:
- Tiny, firm white bumps under the skin (not red, not inflamed)
- Don’t itch, don’t hurt, don’t change much
- Often show up after skin trauma, sun damage, or use of heavy creams
Why regular acne treatments don’t work:
- There’s no infection, inflammation, or oil to target
- Pimple creams, AHAs, or drying treatments can’t dissolve keratin
Treatment options:
- Retinoids (to encourage skin turnover)
- Gentle exfoliation (lactic acid or low-dose glycolic)
- Professional extraction (dermatologist or aesthetician only)
Never try to squeeze milia - they’re too deep and can scar.
4. Keratosis Pilaris (KP)
If the bumps are more like rough patches that feel like sandpaper - especially on your arms, thighs, or cheeks - you’re probably dealing with keratosis pilaris.
What causes it?
- Keratin buildup inside hair follicles
- Usually genetic
- Worsens in dry, cold climates
How it looks:
- Dry, tiny bumps that don’t really "pop"
- Often accompanied by redness or flaking
- Texture stays consistent (no whitehead or head formation)
What helps:
- Urea, lactic acid, or glycolic acid lotions
- Consistent moisturizing
- Gentle exfoliation (no harsh scrubbing)
KP is harmless and not technically acne - and it's notoriously persistent.
A Quick Comparison Table
| Condition | Itchy? | Responds to Acne Actives? | Needs Antifungal Care? | Needs Extraction? |
|---|---|---|---|---|
| Closed Comedones | No | Yes | No | No |
| Fungal Acne | Yes | No | Yes | No |
| Milia | No | No | No | Yes |
| Keratosis Pilaris | No | No | No | No |
When to Reassess Your Routine
If your bumps haven’t changed after:
- 6–8 weeks of exfoliation
- Using salicylic acid or niacinamide regularly
- Switching to non-comedogenic products
…it’s time to stop guessing.
The wrong treatment won’t just waste time - it could damage your barrier and make your skin even harder to read.

Clear Ritual’s Solution: Diagnose → Simplify → Heal
At Clear Ritual, we go beyond “is it acne?”
Our approach helps you understand:
- The root cause of texture or bumps
- What your skin barrier is trying to tell you
- How to reframe skincare from problem-solving to long-term care
We use:
- Gentle cleansers that won’t strip your barrier
- Minimal actives based on your skin type
- Science-backed support for both acne and non-acne texture
Unsure what’s on your face?
Take the [Clear Ritual Skin Test] - and get a plan that doesn’t rely on guesswork.
What If It’s Not Acne?
| Condition | Key Traits | Needs Acne Treatment? |
|---|---|---|
| Closed Comedones | Bumpy, skin-colored, oily | Yes |
| Fungal Acne | Itchy, clustered, sweaty zones | No - needs antifungal |
| Milia | Firm, white, around eyes | No - keratin-based |
| Keratosis Pilaris | Rough, dry, sandpapery | No |
1. How do I know if my bumps are acne or something else?
Acne is usually inflamed, oily, or painful, whereas lookalikes like fungal acne, milia, and keratosis pilaris have distinct patterns such as itching, firmness, or rough texture. Identifying the texture, location, and behaviour helps differentiate them.
2. What does fungal acne look like?
Fungal acne appears as small, uniform, itchy bumps often in clusters on the forehead, hairline, chest, or back. It doesn’t respond to acne treatments and usually requires antifungal care.
3. Why won’t my closed comedones go away even with acne products?
Closed comedones can persist due to occlusive skincare, dead skin buildup, or improper exfoliation. If bumps don’t improve after 6–8 weeks, they may not be closed comedones at all, but fungal acne, milia, or KP.
4. Can I pop or extract milia at home?
No — milia are hard keratin cysts located under the skin and cannot be popped. Only a dermatologist or aesthetician can safely extract them.
5. What’s the best way to treat keratosis pilaris (KP)?
KP responds best to moisturisers with urea, lactic acid, or glycolic acid. Consistent gentle exfoliation helps, while acne spot treatments will not improve KP.
Editorial Standards
Clear Ritual has Strict sourcing guidelines to ensure our content is accurate and current. We rely on peer-reviewed studies, academic research institutions, and medical associations. We strive to use primary sources and refrain from using tertiary references. See a mistake? Learn More about our Editorial Standards.

