Papules Acne: Causes, Symptoms, Treatment & Prevention

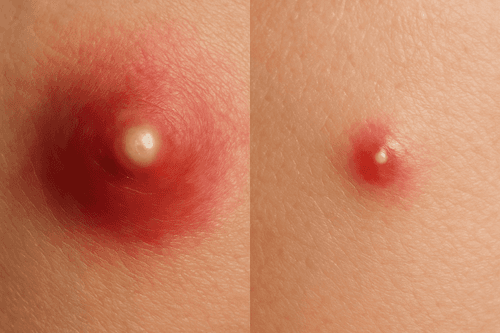
Papules acne is a small, red or purple-coloured, inflamed acne bumps with no pus-filled tips (white or yellow centre). It forms when your skin pores are clogged with sebum oil, dead skin cells, and bacteria. In some cases, papule acne is also triggered by hormonal changes and excessive stress. Over-the-counter medicines containing salicylic acid and benzoyl peroxide, as well as certain home remedies, can help reduce symptoms. If OTC medicines fail and the condition becomes severe over time, consult your dermatologist for further assistance.
You noticed a few red bumps on your face and chose to ignore them, thinking they were another regular case of acne. The day passed, but instead of disappearing, the acne seemed to multiply. Now, if this sounds familiar to you even slightly, you might be dealing with papules acne. Don’t worry, the word might sound scary, but the treatment is simpler than you can imagine. Here’s everything you need to know about papules acne before you know how to treat it.
What Is Papules Acne?
Acne papules are small, inflamed pimples that are either red or purple in colour. They can also be skin colored bumps. They look different from white or yellow pimples that show up every now and then. Acne papules typically affect teenagers with hormonal fluctuations, but in some cases, they can also affect people in their 20s and 30s. They usually appear on the nose, chin, forehead, neck, and the back of your body.
Symptoms of Papules Acne
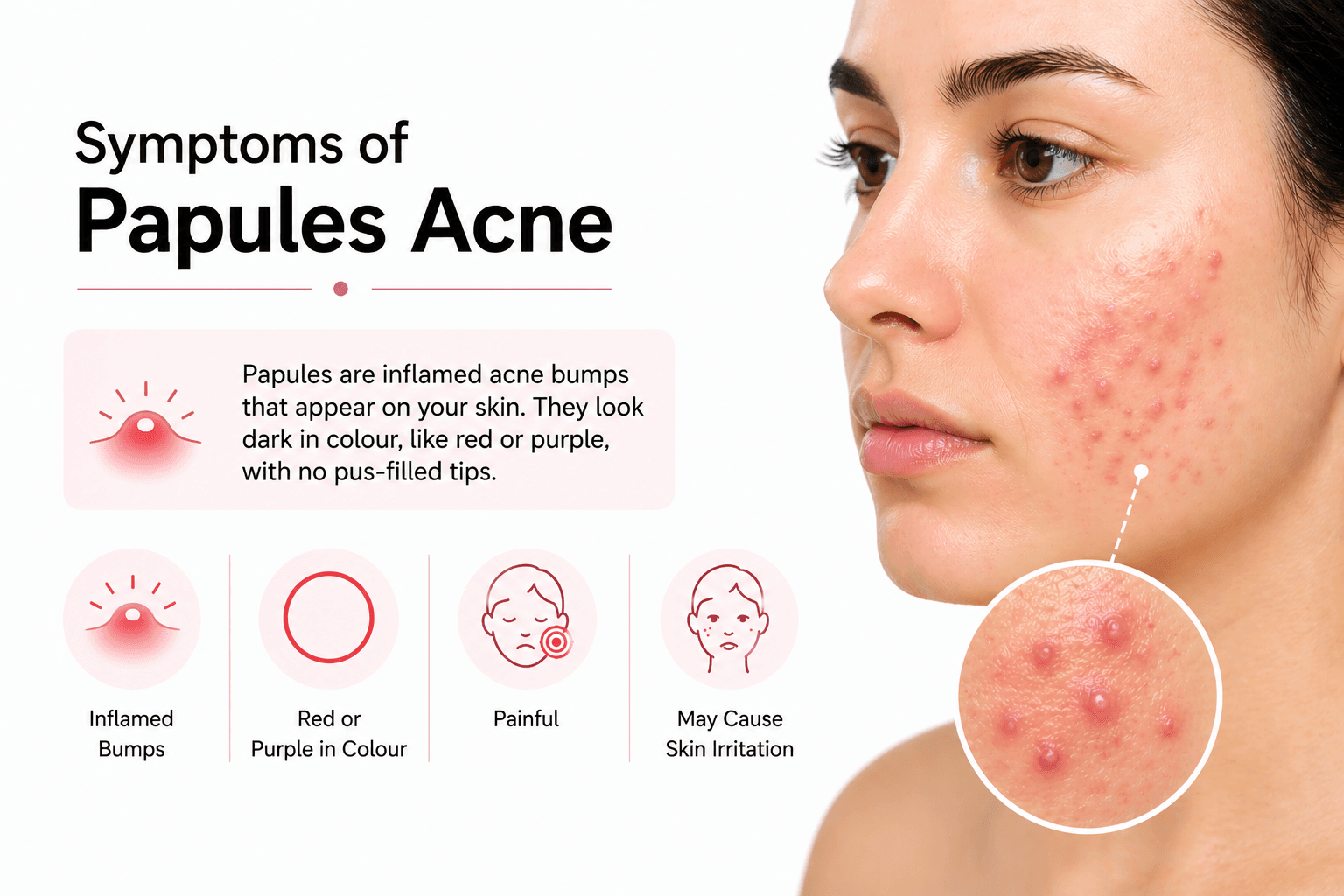
Papules are inflamed acne bumps that appear on your skin. They look dark in colour, like red or purple, with no pus-filled tips. It is a painful acne type that can also cause skin irritation.
Causes of Papules Acne
The main causes of papular acne are your skin follicles being clogged with excess oil, dead skin, and bacteria. A fluctuation in androgens (sex hormones) can also be the cause of papule acne.
Another reason for papular acne is stress, as well as poor dietary and lifestyle habits, such as consuming excessive amounts of sugary products, fast food and dairy products.
Diagnosis of Papules Acne
Papular acne is easily recognisable by its reddish, inflamed lesions. If you are taking professional help, your doctor may ask you these questions:
- Have you been under a lot of stress recently?
- Did any of your parents or ancestors have papules acne?
- What does your daily routine look like?
- What do you eat in a day?
- Does papular acne appear during your period or as it approaches?
Answering these questions helps your dermatologist determine the cause of your recurring papules acne and treat the condition effectively.
Papules Acne Treatment & Management
Understanding how to treat papules acne will help you relieve mild skin acne. You can use non-prescription medicines such as azelaic acid, benzoyl peroxide, retinoids, and salicylic acid to soothe the papules acne symptoms.
If you don’t find these medicines helpful, consulting your doctor is your only option. Your dermatologist may recommend antibiotics, anti-androgens, dapsone, and oral contraceptives (birth control pills) to treat papular acne.
How to Prevent Papules Acne?
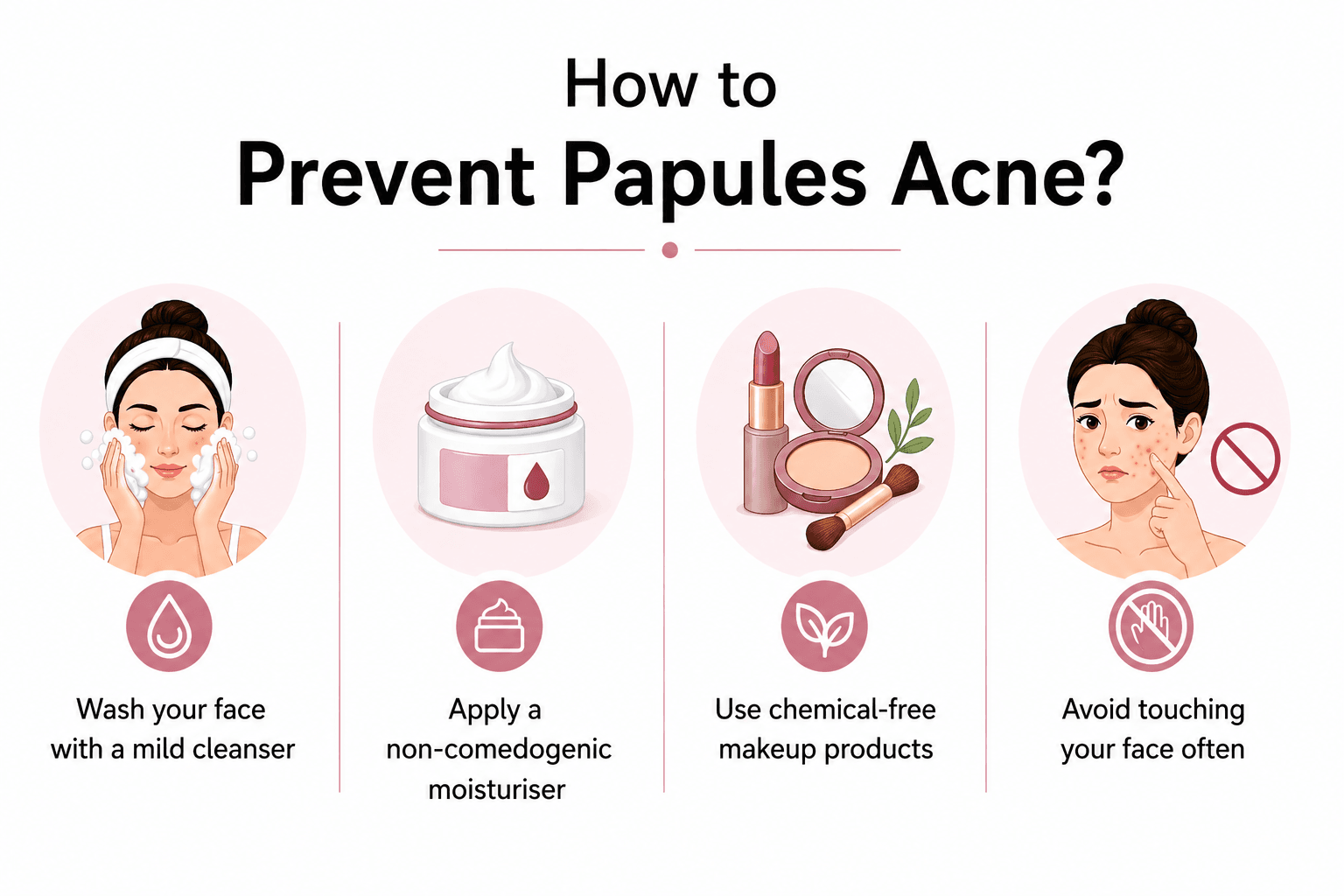 Everyone wants clear skin, right? Papules acne is a common condition and is easily manageable. But knowing how to prevent it will certainly help you maintain clearer and healthier skin.
Everyone wants clear skin, right? Papules acne is a common condition and is easily manageable. But knowing how to prevent it will certainly help you maintain clearer and healthier skin.
- Wash your face with a mild cleanser
- Apply a non-comedogenic moisturiser
- Use chemical-free makeup products
- Avoid touching your face often
These are tips to prevent recurring papules acne on your skin. Besides these methods, ensure you wash your hair at least twice a week, as unwashed hair contains bacteria that can also cause regular acne or papules.
Home Remedies for Papules Acne
Internal cleansing is the first step toward clear, acne-free skin. Try these home remedies listed below to achieve a healthier glow.
Topical Treatments (Apply to skin only)
- Apple cider vinegar: Mix apple cider vinegar with water, then apply it to breakouts using a cotton applicator.
- Green tea leaves: Mix dry green tea leaves with water, then massage the mixture onto your papular acne in a circular motion for a few seconds.
- Honey: Use honey as a natural mask to soothe inflamed areas.
- Lemon juice: Apply a small amount of lemon juice to your papules, then rinse it off after a minute.
- Tea tree oil: Apply tea tree oil to your breakouts and rub it gently for a few seconds.
While home remedies can be effective, you should consult a dermatologist if you don't see visible results. It is important to treat papular acne early, as leaving it unchecked can lead to permanent skin scarring and deeper inflammation.
Papules vs Other Types of Acne
Identifying your acne type correctly is crucial for choosing the right treatment. This table highlights the key differences between papules and other common acne variants.
| Type | Appearance | Cause | Pain and inflammation | Risk of scarring |
|---|---|---|---|---|
| Papules | Looks like red, inflamed bumps and often painful | Papules occur when pores are blocked by excess oil, dead skin cells, and bacteria. It can also be caused by hormonal changes and excessive stress. | Inflammatory and painful | Moderate |
| Blackheads | Looks like a small dark spot | It is caused when your clogged skin pores are exposed to air and oxidise | Non-inflammatory and painless | Low |
| Whiteheads | Looks like a small white spot | It is caused when your follicles are clogged with dead skin cells and bacteria | Non-inflammatory and painless | Low |
| Nodules | Looks like a large bump beneath the skin surface | Nodules are caused by inflammation and deep infection within the skin follicles | Inflammatory and painful | High |
| Pustules | Looks like red-inflamed bumps with pus-filled (white and yellow centre) | They are caused by inflammation in papules that worsen and create white fluids | Inflammatory and painful | Moderate |
| Cysts | Looks like a large, soft, fluid-filled bump | Cysts are caused by severe infection within skin pores | Severe, Inflammatory and painful | Very High |
Once you know the difference between the acne types, you will know which treatment you need to relieve your papules acne symptoms.
Clear Ritual’s Perspective on Papules Acne & Its Treatment
At Clear Ritual, the focus goes beyond quick fixes. It identifies the root cause of your skin issues and provides a permanent solution. See, acne has several types, and papular acne is one of them. While it is possible to treat breakouts with over-the-counter and prescription medicines such as antibiotics, anti-androgens, benzoyl peroxide, and azelaic acid, these may fail to address the core cause if acne occurs frequently. Papules happen when follicles are clogged with bacteria, dead skin cells, and excess oil. Other contributing factors include stress, hormonal imbalances, and a poor diet.
Understanding the cause of your acne provides deeper insight into the areas you need to improve. A Clear Ritual Skin Test can help you identify the root cause and provide a holistic treatment plan. The goal is to relieve symptoms while addressing the source, ensuring clearer skin in the long run.
Frequently Asked Questions
Q1. Are papules contagious?
Papular acne is a non-contagious skin condition, meaning it does not spread from one person to another or from one part of the body to another.
Q2. How can I manage papules acne?
Using products with active ingredients such as benzoyl peroxide and salicylic acid can help you manage and treat papular acne. Additionally, wash your face with a gentle cleanser and use sunscreen to protect inflamed skin from UV rays.
Q3. What is the difference between a papule and a pustule?
Papule acne is red, inflamed acne without pus, often painful. And pustule acne looks inflamed, but it is pus-filled. They both leave a moderate level of scarring on your skin.
Q4. Is papule acne harmful?
Papules acne is a common form of inflamed acne, and is not dangerous. Though not harmful, it can be painful and leave scars on the face.
Q5. Do papules go away on their own?
When papules go away depends on your skin type and the severity of the condition. Normally, you can relieve the papule's symptoms with over-the-counter medicines, and if it doesn’t heal, you should consult your dermatologist for treatment.
Reference Links
Editorial Standards
Clear Ritual has Strict sourcing guidelines to ensure our content is accurate and current. We rely on peer-reviewed studies, academic research institutions, and medical associations. We strive to use primary sources and refrain from using tertiary references. See a mistake? Learn More about our Editorial Standards.