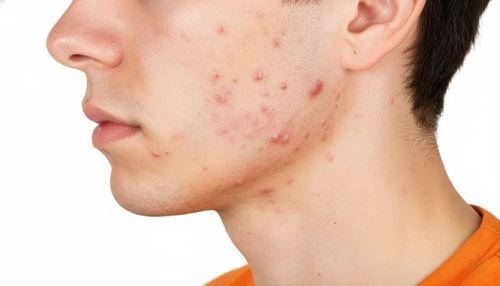
How to Treat Cystic Acne on Cheeks and Forehead Correctly?

Cystic acne on the cheeks and forehead is a deep, inflammatory lesion, one of the most severe forms of acne. Unlike surface-level spots, cystic acne occurs when the pores, clogged with oil and dead skin cells, become infected with bacteria after the wall of a clogged follicle ruptures, spilling its contents into the surrounding dermis.
To treat cystic acne on the cheeks and forehead, avoid harsh, drying products. Instead, focus on anti-inflammatory ingredients, or use doctor-prescribed medications, and avoid picking at the acne to prevent permanent scarring.
Some lifestyle habits, like frequently changing pillowcases and not constantly touching the face, and hygiene practices, may help prevent inflammation from becoming severe. Using over-the-counter treatments can help manage acne and keep pores clean. Cystic acne is usually stubborn and doesn't go away on its own. You need to consult a dermatologist to treat it with the right medications and treatments.
Cystic Acne on Cheeks and Forehead
Cystic acne on the cheeks and forehead often happens if you rest your face on your hands, do not clean your mobile screen before a call, rub against pillowcases, use hair products, have heavy bangs on the forehead, sweat a lot, or wear tight hats and headbands.
Friction and pressure cause acne mechanica by occluding follicles and triggering keratinocyte hyperproliferation. Bacteria are not physically pushed in; an anaerobic environment allows resident C. acnes to increase.
Cystic acne can be painful and large because they develop deep under the skin. If not treated correctly, they can lead to severe breakouts and leave permanent scars. Cystic acne can cause deep tissue damage, disrupt collagen, and worsen inflammation. Cystic acne on the cheeks predominantly causes atrophic (ice-pick, boxcar, rolling) scars. Hypertrophic and keloid scars are less common but can occur on the chest or back.
Causes of Cystic Acne on Cheeks
Cystic acne on the cheeks is caused by primary triggers like hormonal changes and genetics, and is worsened by physical triggers that push bacteria into the pores. The main causes of developing cystic acne on the cheeks are:
-
Hormonal Fluctuations: During menopause, oestrogen drops while androgens may remain relatively elevated, the ratio shifts, not the androgen level itself. Pregnancy also does not always cause a spike; some women see improvement. Androgens (particularly DHT) bind to receptors in sebaceous glands, leading to increased sebum production.
-
Genetics: People with a family history of cystic acne are more likely to develop it. However, lifestyle habits, hygiene, and precautions may help in avoiding the development of deep, painful cysts.
-
Friction & Pressure: Holding mobile phones directly against your face or rubbing your skin against dirty pillowcases traps and pushes sweat, oil, and bacteria, which can penetrate the skin.
-
Heavy Products: Using comedogenic makeup products, heavy, oily creams, and dirty makeup tools can clog pore openings and transfer bacteria, both of which can trigger breakouts.
Cystic Acne on Cheeks Treatment
Cystic acne treatment requires a more targeted approach than superficial pustules or surface-level spots. Always consult a dermatologist before starting new treatments. If you are looking for spot treatments that work well on cystic acne, you should try:
-
Ice or Cold Compress: Wrap an ice cube in a soft cotton cloth and gently press it against the cysts for a few minutes to help reduce swelling, inflammation, and pain.
-
Targeted Spot Treatment: Use a pea-sized amount of benzoyl peroxide or salicylic acid, then dab it onto surface-level spots. For deep cysts, they can help prevent new clogging around the area, but do not resolve the cyst itself.
-
Pimple Patches: Using pimple patches keeps the cyst protected from bacteria and helps protect the skin when you apply makeup over it.
Cystic Acne on Forehead Causes
People with oily or combination skin can develop excess oil in the T-zone, making their foreheads prone to cystic acne. Hair care residue is a leading cause of cystic acne on the forehead. Using heavy hair products like hair gels, leave-in sprays, pomades, and oils can reach the forehead and clog pores. Dandruff flakes can settle along the hairline, clogging pores and contributing to breakouts there.
Cystic Acne on Forehead Treatment
Cystic acne on the forehead needs to be treated with a dermatologist-guided approach, as physically removing the cysts is not recommended. Some clinically safe options to treat cystic acne on the forehead are:
-
Corticosteroid Injections: This is a professional treatment a dermatologist recommends for sudden, painful cysts, designed to shrink them and reduce inflammation within 24 to 72 hours.
-
Prescription Retinoids: Prescription retinoids like tretinoin or tazarotene help regulate skin cell turnover and prevent pore clogging.
-
Oral Medications: Doctors prescribe oral antibiotics (such as doxycycline) to reduce bacterial load and inflammation, or isotretinoin for cases that do not respond to other treatments.
-
Over-the-counter Options: Salicylic acid, benzoyl peroxide, or sulfur are common spot treatments effective for cystic acne.
Clear Ritual’s Perspective on Cystic Acne on Cheeks and Forehead
Clear Ritual recommends a gentle yet targeted approach that calms inflammation and clears pores without relying on harsh products or physical force. The Clear Ritual Skin Test helps you identify the root cause of your breakouts and address them effectively.
We advise refraining from aggressive physical removal of the cysts or from using harsh chemicals that dry out the skin or worsen inflammation. For persistent cystic acne, dermatologist-led treatments remain the most reliable way to heal without causing lasting skin damage.
Frequently Asked Questions
What causes cystic acne on the cheeks and forehead?
The primary causes of cystic acne on cheeks and forehead include deep inflammation triggered by excess sebum, bacteria, hormonal shifts, and friction.
How to treat cystic acne on the forehead?
To treat cystic acne on the forehead, avoid product buildup on your forehead and hairline, use products that help control excess sebum, and target healing of cysts.
Why are you breaking out on your cheeks, chin, and forehead?
If you are breaking out on your cheeks, chin, and forehead at the same time, it might be due to internal and external triggers, inflammation, or excess sebum production. Getting it diagnosed by a dermatologist can help you understand its root cause and treat it effectively.
How do Koreans treat cystic acne?
The Korean beauty (K-beauty) approach to cystic acne emphasises skin barrier protection and gentle hydration over aggressive stripping of moisture, followed by dermatological interventions and soothing treatments.
References
https://my.clevelandclinic.org/health/diseases/21737-cystic-acne
Editorial Standards
Clear Ritual has Strict sourcing guidelines to ensure our content is accurate and current. We rely on peer-reviewed studies, academic research institutions, and medical associations. We strive to use primary sources and refrain from using tertiary references. See a mistake? Learn More about our Editorial Standards.